Submitted:
20 March 2024
Posted:
22 March 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Epidemiology
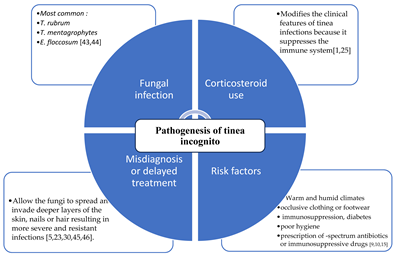
3. Pathogenesis
4. Clinical Features
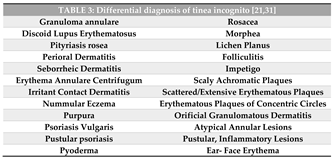
5. Diagnosis
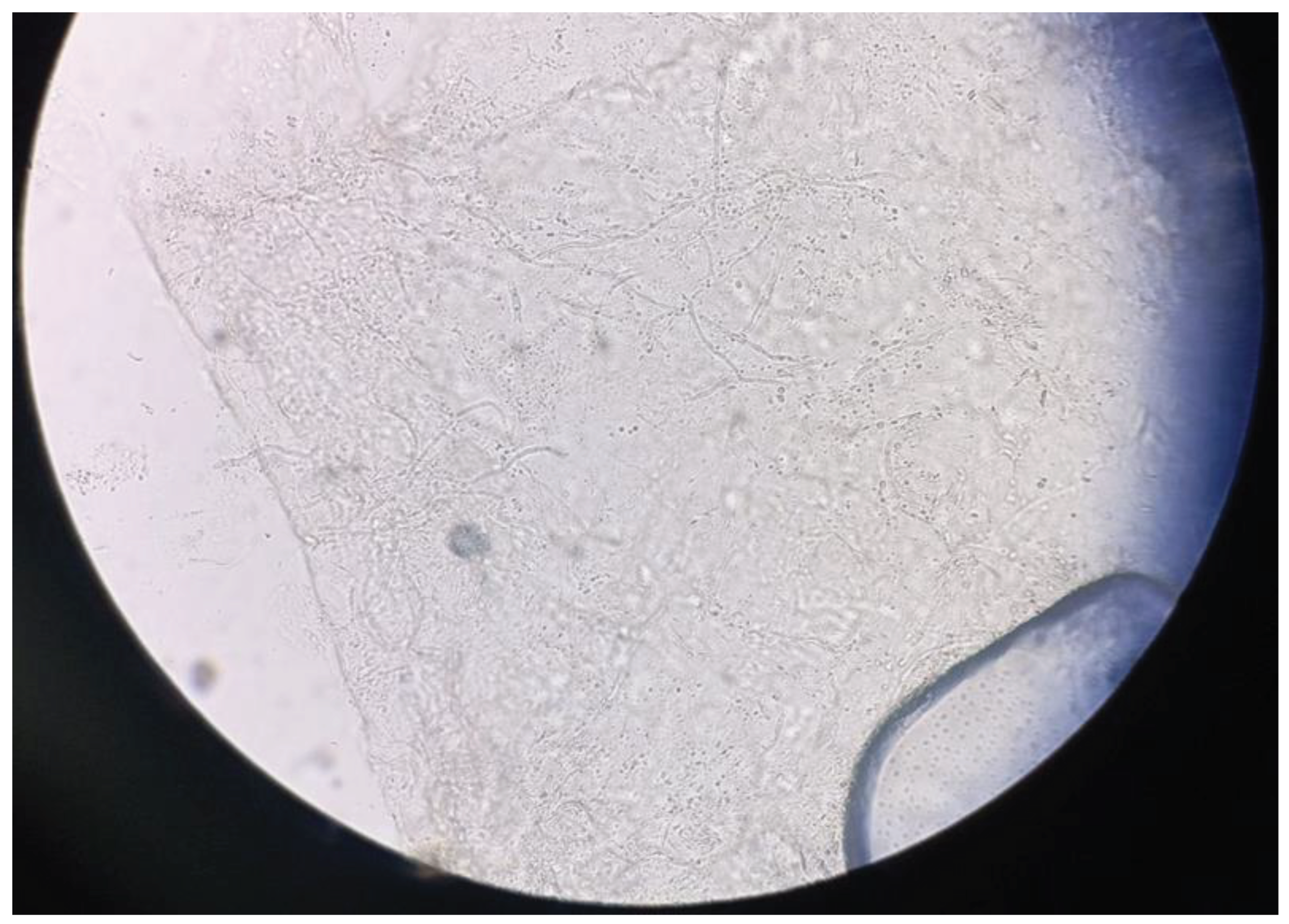
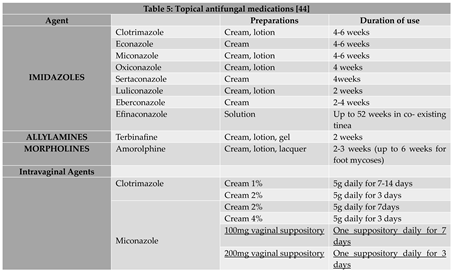
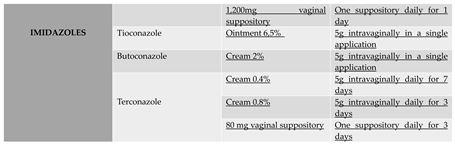
6. Treatment
7. Recurrence
8. Financial Considerations
9. Conclusion
Author Contributions
Funding
Ethics statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ive FA, Marks R. Tinea incognito. Br Med J 1968, 3, (149-152.
- Simmons I. Tinea Incognito. In Diagnosis and Treatment of Cutaneous Fungal Infections for General Practitioners. Sandoz Satellite Symposium of the 12th Congress International Society for Human and Animal Mycology, SARMEA , 1994.
- Jagadeesan S, Sreekumar S, Sajini L, Binu A, Das A, The economic burden of topical corticosteroid use in dermatophytosis: A cost of illness analysis of steroid-modified vs steroid-naïve dermatophytosis. Clin Exp Dermatol 2023, IIad135. [CrossRef]
- Atzori L, Pau M, Aste N, Aste N. Dermatophyte infections mimicking other skin diseases: A 154-person case survey of tinea atypica in the district of Cagliari (Italy). Int J Dermatol 2012, 51, 410-5.
- Siddaiah N, Erickson Q, Miller G, Elston DM. Tacrolimus-induced tinea incognito. Cutis 2004, 73, 237-8.
- Crawford KM, Bostrom P, Russ B, Boyd J. Pimecrolimus-induced tinea incognito. Skinmed 2004, 3, 352-3.
- Krajewska-Kulak E, Niczyporuk W, Lukascuk C, Bartoszewicz M, Roszkowska I, Edyta M.. Difficulties in diagnosing and treating tinea in adults at the Department of Dermatology in Bialystok (Poland). Dermatol Nurs 2003, 15, 527-30.
- Kim MW, Park HS, Bae JM, Yoon HS, Cho S. Tinea Incognito with Folliculitis-Like Presentation: A Case Series. Ann Dermatol 2018, 30, 97-9. [CrossRef]
- Dutta B, Rasul ES, Boro B. Clinico-epidemiological study of tinea incognito with microbiological correlation. Indian J Dermatol Venereol Leprol 2017, 83, 326-31. [CrossRef]
- Gawdzik A, Nowogrodzka K, Hryncewicz-Gwóźdź A, Maj J, Szepietowski J, Jankowska-Konsur A. Epidemiology of dermatomycoses in southwest Poland, years 2011–2016. Postepy Dermatol Alergol 2019, 36, 604-608. [CrossRef]
- Samer Dhaher. Tinea incognito: Clinical perspectives of a new imitator.Dermatol Reports. 2020 Jun 25; 12(1): 8323. [CrossRef]
- Thomas Stringer, Julia K. Gittler, Seth J. Orlow. Tinea Incognito in an Urban Pediatric Population. Cutis. 2018 November;102(5):370-372.
- J. del Boz, V. Crespo, F. Rivas-Ruiz, M. de Troya. Tinea incognito in children: 54 cases. Mycoses 2011 Volume54, Issue3 ,pages 254-258. [CrossRef]
- Abed Ali FAH, Jawad K, Al-Janabi A, Alhattab MK. Prevalence of dermatophyte fungal infection in Hillah, Iraq. Int J Chem Tech Res 2017, 10, 827-37.
- Yee G, Al Aboud AM. Tinea Corporis. In: StatPearls [Internet]. Treauser Island (FL): StatPearls Publishing; 2023.
- King RD, Khan HA, Foye JC, Greenberg JH, Jones HE. Transferrin, iron, and dermatophytes. I. Serum dermatophyte inhibitory component definitively identified as unsaturated transferrin. J Lab Clin Med 1975, 86, 204-12.
- Wollina U, Hansel G, Koch A, Abdel-Naser MB. Topical pimecrolimus for skin disease other than atopic dermatitis. Expert Opin Pharmacother. 2006, 7, 1967-75. [CrossRef]
- Singh A, Masih A, Khurana A, Singh PK, Gupta M, Hagen F, Meis JF, Chowdhary A. High terbinafine resistance in Trichophyton interdigitale isolates in Delhi, India harbouring mutations in the squalene epoxidase gene. Mycoses 2018, 61, 477-84.
- Dabas Y, Xess I, Singh G, Pandey M, Meena S. Molecular identification and antifungal susceptibility patterns of clinical dermatophytes following CLSI and EUCAST guidelines. J Fungi (Basel) 2017, 3, 17. [CrossRef]
- Rudramurthy SM, Shankarnarayan SA, Dogra S, Shaw D, Mushtaq K, Paul RA, Narang T, Chakrabarti A. Mutation in the Squalene Epoxidase Gene of Trichophyton interdigitale and Trichophyton rubrum Associated with Allylamine Resistance. Antimicrob Agents Chemother 2018, 62, e02522-17. [CrossRef]
- Kim WJ, Kim TW, Mun JH, Song M, Kim HS, Ko HC, et al. Tinea incognito in Korea and its risk factors: Nine-year multicenter survey. J Korean Med Sci 2013, 28, 145-51. [CrossRef]
- Arun B, Remya VS, Sheeba PM, Kokkayil P. Mycological study on incidence of tinea incognito in a tertiary hospital. Med Pulse-International Medical Journal 2015, 2, 649-51.
- Romano C, Maritati E, Gianni C. Tinea incognito in Italy: A 15-year survey. Mycoses 2006, 49, 383-7. [CrossRef]
- Turk BG, Taskin B, Karaca N, Sezgin AO, Aytimur D. Clinical and mycological analysis of twenty-one cases of tinea incognita in the Aegean region of Turkey: A retrospective study. Acta Dermatovenerol Croat 2013, 21, 93-8.
- Pustisek N, Skerlev M, Basta-Juzbasic A, Lipozencic J,Marinovic B, Bukvic-Mokos Z. Tinea incognito caused by Trichophyton mentagrophytes. Acta Dermatovenerol Croat 2001, 9, 283-6.
- Arenas R., Moreno-Coutiño G., Vera L., Welsh O. Tinea incognito. Clin Dermatol 2010, 28, 137-9.
- Gorani A, Schiera A, Oriani A. Case report. Rosacea-like tinea incognito. Mycoses 2002, 45, 135-7.
- Romano C, Asta F, Massai L. Tinea incognito due to Microsporum gypseum in three children. Pediatr Dermatol 2000, 17, 41-4. [CrossRef]
- Faergemann J, Fredriksson T, Herczka O, Krupicka P, Bjorklund KN, Sjokvist M. Tinea incognito as a source of an "epidemic" of Trichophyton violaceum infections in a dermatologic ward. Int J Dermatol 1983, 22, 39-40. [CrossRef]
- Feder Jr HM. Tinea incognito misdiagnosed as erythema migrans. N Engl J Med 2000, 343, 69.
- Ansar A, Farshchian M, Nazeri H, Ghiasian SA. Clinico-epidemiological and mycological aspects of tinea incognito in Iran: A 16-year study. Med Mycol J 2011, 52, 25-32. [CrossRef]
- Naglot A, Shrimali DD, Nath BK, Gogoi HK, Veer V, Chander J, Tewari R. Recent trends of dermatophytosis in Northeast India (Assam) and interpretation with published studies. Int J Curr Microbiol Appl Sci 2015, 4, 111-20.
- Sahai S, Mishra D. Change in spectrum of dermatophytes isolated from superficial mycoses cases: First report from Central India. Indian J Dermatol Venereol Leprol 2011, 77, 335-6.; [CrossRef]
- J Del Boz J, Crespo V, Rivas-Ruiz F, De Troya M. Tinea incognito in chil dren: 54 cases. Mycoses 2011, 54, 254-8. [CrossRef]
- Johnson RA: HIV disease: mucocutaneous fungal infections in HIV disease. Clin Dermatol 2000, 18, 411-22.
- Galhardo MCG, Wanke B, Reis RS, Oliveira LA, Valle ACF. Disseminated dermatophytosis caused by Microsporum gypseum in an AIDS patient: response to terbinafin and amorolfine. Mycoses 2004, 47, 238-41. [CrossRef]
- Luque AG, Biasoli MS, Sortino MA, Lupo SH, Bussy RF. Atypical tinea corporis caused by Microsporum gypseum in a subject with acquired immune deficiency syndrome. J Eur Acad Dermatol Venereol 2001, 15, 374-5.
- Porro AM, Yoshioka MC, Kaminski SK, Palmeira M do C, Fischman O, Alchorne MM. Disseminated dermatophytosis caused by Microsporum gypseum in two patients with the acquired immunodeficiency syndrome. Mycopathologia 1997, 137, 9-12. [CrossRef]
- Prochnau A, de Almeida HL Jr, Souza PRM, Vetoratto G, Duquia RP, Defferrari R. Scutular tinea of the scrotum: report of two cases. Mycoses 2005, 48, 162-4.
- Romano C, Massai L, Gallo A, Fimiani M: Microsporum gypseum infection in the Siena area in 2005–2006. Mycoses 2009, 52, 67-71.
- Jensen JM, Pfeiffer S, Akaki T, Schröder JM, Kleine M, Neumann C, Proksch E, Brasch J. Barrier function, epidermal differentiation and human b-defensin 2expression in tinea corporis. J Invest Dermatol 2007, 127, 1720-7.
- Gupta AK, Konnikov N, MacDonald P, Rich P, Rodger NW, Edmonds MW, McManus R, Summerbell RC. Prevalence and epidemiology of toenail onychomycosis in diabetic subjects: A multicentre survey. Br J Dermatol 1998, 139, 665-71. [CrossRef]
- Weitzman I, Summerbell RC. The dermatophytes. Clin Microbiol Rev 1995, 8, 240-59.
- Sahoo AK, Mahajan R. Management of tinea corporis, tinea cruris, and tinea pedis: A comprehensive review. Indian Dermatol Online J 2016, 7, 77-86. [CrossRef]
- Guenova E, Hoetzenecker W, Schaller M, Rocken M, Fierlbeck G. Tinea incognito hidden under apparently treatment- resistant pemphigus foliaceus. Acta Derm Venereol 2008, 88, 276-7. [CrossRef]
- Solomon BA, Glass AT, Rabbin PE. Tinea incognito and “over-the-counter” potent topical steroids. Cutis 1996, 58, 295-6.
- Gupta AK, Ryder JE, Chow M, Cooper EA. Dermatophytosis: The management of fungal infections. Skinmed 2005, 4, 305-10.
- Park YW, Choi JW, Paik SH, Kim DY, Jin SP, Park HS, Yoon HS, Cho S. Tinea incognito simulating herpes simplex virus infection. Ann Dermatol 2014, 26, 267-9. [CrossRef]
- Sardana K, Gupta A, Aastha M, Mathachan SR. Immunopathogenesis of Dermatophytoses and Factors Leading to Recalcitrant Infections. Indian Dermatol Online J 2021, 12, 389-99. [CrossRef]
- Novick NL, Tapia L, Bottone EJ. Invasive trichophyton rubrum infection in an immunocompromised host. Case report and review of the literature. Am J Med 1987, 82, 321-5. [CrossRef]
- Grossman ME, Pappert AS, Garzon MC, Silvers DN. Invasive Trichophyton rubrum infection in the immunocompromised host: report of three cases. J Am Acad Dermatol 1995, 33, 315-8. [CrossRef]
- Erbagci Z. Topical therapy for dermatophytoses: should corticosteroids be included? Am J Clin Dermatol 2004, 5, 375-84.
- Lekkas D, Ioannides D, Lazaridou E, Lallas A, Apalla Z, Vakirlis E, Johr R, Errichetti E, Kyrgidis A, Sotiriou E. Dermatoscopy of tinea corporis. J Eur Acad Dermatol Venereol 2020, 34, e278-e280.
- Slowinska M, Rudnicka L, Schwartz RA, Kowalska-Oledzka E, Rakowska A, Sicinska J, Lukomska M, Olszewska M, Szymanska E. Comma hairs—A dermoscopic marker for tinea capitis. A rapid diagnostic method. J Am Acad Dermatol 2008, 59, S77-9.
- Piraccini BM, Balestri R, Starace M, Rech G. Nail digital dermoscopy (Onychoscopy) in the diagnosis of onychomycosis. J Eur Acad Dermatol Venereol 2013, 27, 509-13. [CrossRef]
- Rajagopalan M, Inamadar A, Mittal A, Miskeen AK, Srinivas CR, Sardana K, Godse K, Patel K, Rengasamy M, Rudramurthy S, Dogra S. Expert Consensus on The Management of Dermatophytosis in India (ECTODERM India). BMC Dermatol 2018, 18, 6. [CrossRef]
- Pihet M, Le Govic Y. Reappraisal of Conventional Diagnosis for Dermatophytes. Mycopathologia 2017, 182, 169-180. [CrossRef]
- Kurade SM, Amladi SA, Miskeen AK. Skin scraping and a potassium hydroxide mount. Indian J Dermatol Venereol Leprol 2006, 72, 238-41. [CrossRef]
- Ahmad MR, Javed I, Mushtaq S. Evaluation of Chicago sky blue stain against Potassium Hydroxide-Dimethyl Sulfoxide wet mount in the identification of dermatophytes. J Fatima Jinnah Med Univ 2020, 14, 83-86. [CrossRef]
- Lasseter G, Palmer M, Morgan J, Watts J, Yoxall H, Kibbler C, McNulty C. Members of the HPA GP Microbiology Laboratory Use Group Developing best practice for fungal specimen management: Audit of UK microbiology laboratories. Br J Biomed Sci 2011, 68, 197-202.
- Ovrén E, Berglund L, Nordlind K, Rollman O. Dermatophytosis: Fluorostaining enhances speed and sensitivity in direct microscopy of skin, nail and hair specimens from dermatology outpatients. Mycoses 2016, 59, 436-41. [CrossRef]
- Sumathi S, Pandit VS, Patil S, Adavi V. A cross sectional clinicomycological study of dermatophytosis in a tertiary care hospital, North Karnataka, India. IP Int J Med Microbiol Trop Dis 2018, 4, 166-70. [CrossRef]
- Singh J, Zaman M, Gupta AK. Evaluation of microdilution and disk diffusion methods for antifungal susceptibility testing of dermatophytes. Med Mycol 2007, 45, 595-602. [CrossRef]
- Park YW, Kim DY, Yoon SY, Park GY, Park HS, Yoon HS, Cho S. ‘Clues’ for the histological diagnosis of tinea: How reliable are they? Ann Dermatol 2014, 26, 286-8.
- Navarrete-Dechent C, Bajaj S, Marghoob AA, Marchetti MA. . Rapid diagnosis of tinea incognito using handheld reflectance confocal microscopy: a paradigm shift in dermatology? Mycoses 2015, 58, 383-6.
- Li HC, Bouchara JP, Hsu MML, Barton R, Su S, Chang TC. Identification of dermatophytes by sequence analysis of the rRNA gene internal transcribed spacer regions. J Med Microbiol 2008, 57, 592-600. [CrossRef]
- Friedman D, Friedman PC, Gill M. Reflectance confocal microscopy: An effective diagnostic tool for dermatophytic infections. Cutis 2015, 95, 93-7.
- Turan E, Erdemir AT, Gurel MS, Yurt N. A new diagnostic technique for tinea incognito: In vivo reflectance confocal microscopy. Report of five cases. Skin Res Technol 2013, 19, e103-7.
- Cowen LE, Sanglard D, Howard SJ, Rogers PD, Perlin DS. Mechanisms of antifungal drug resistance. Cold Spring Harb Perspect Med 2014, 5, a019752. [CrossRef]
- De Sousa MGT, Santana GB, Criado PR, Benard G. Chronic widespread dermatophytosis due to Trichophyton rubrum: A syndrome associated with a Trichophyton-specific functional defect of phagocytes. Front Microbiol 2015, 6, 801. [CrossRef]
- Sugita K, Kabashima K, Atarashi K, Shimauchi T, Kobayashi M, Tokura Y. Innate immunity mediated by epidermal keratinocytes promotes acquired immunity involving Langerhans cells and T cells in the skin. Clin Exp Immunol 2007, 147, 176-83. [CrossRef]
- Sardana K, Kaur R, Arora P, Goyal R, Ghunawat S. Is antifungal resistance a cause for treatment failure in dermatophytosis: A study focused on tinea corporis and cruris from a tertiary centre? Indian Dermatol Online J 2018, 9, 90-5.
- Marconi VC, Kradin R, Marty FM, Hospenthal DR, Kotton CN. Disseminated dermatophytosis in a patient with hereditary hemochromatosis and hepatic cirrhosis: Case report and review of the literature. Med Mycol 2010, 48, 518-27. [CrossRef]
- Hay RJ, Baran R. Deep dermatophytosis: Rare infections or common, but unrecognised, complications of lymphatic spread? Curr Opin Infect Dis 2004, 17, 77-9.
- Rouzaud C, Hay R, Chosidow O, Dupin N, Puel A, Lortholary O, Lanternier F. Severe dermatophytosis and acquired or innate immunodeficiency: A review. J Fungi (Basel) 2015, 2, 4. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).