Submitted:
26 April 2024
Posted:
26 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
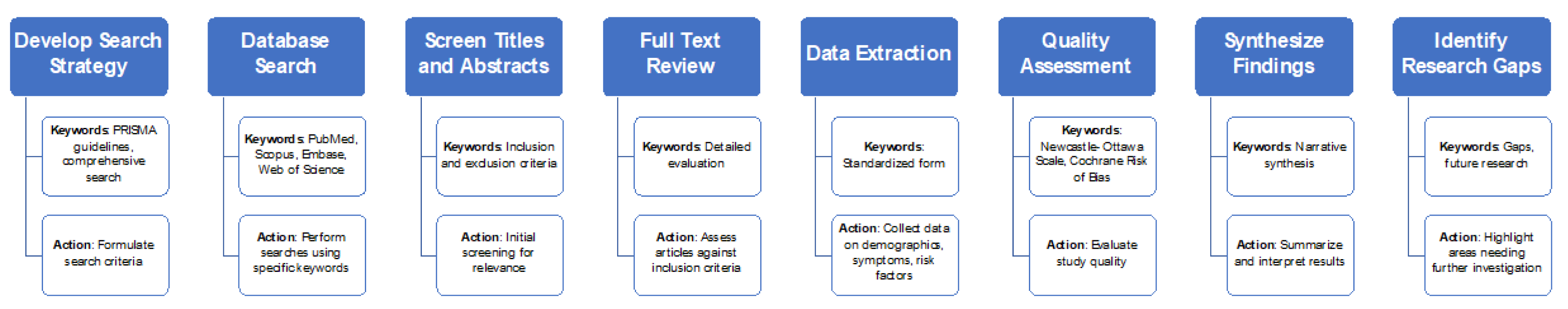
2. Materials and Methods
3. Results
3.1. Symptoms of Long COVID
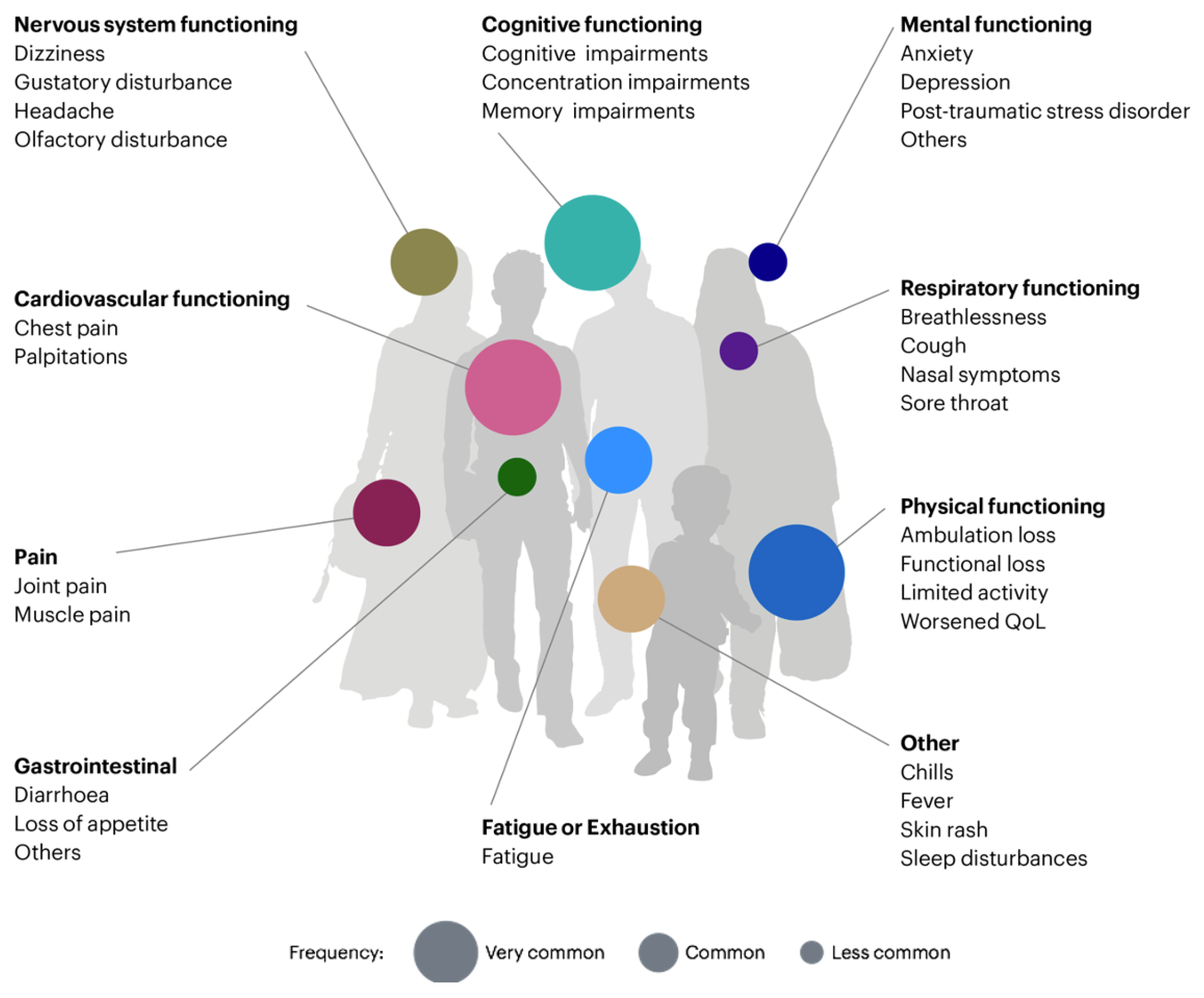
3.1.1. Typical Symptoms of Long COVID
3.1.2. Duration of the Long COVID in the Patient
3.2. Risk Factors and Physiological Mechanisms that Trigger Long COVID
3.2.1. Risk Factors for Long COVID
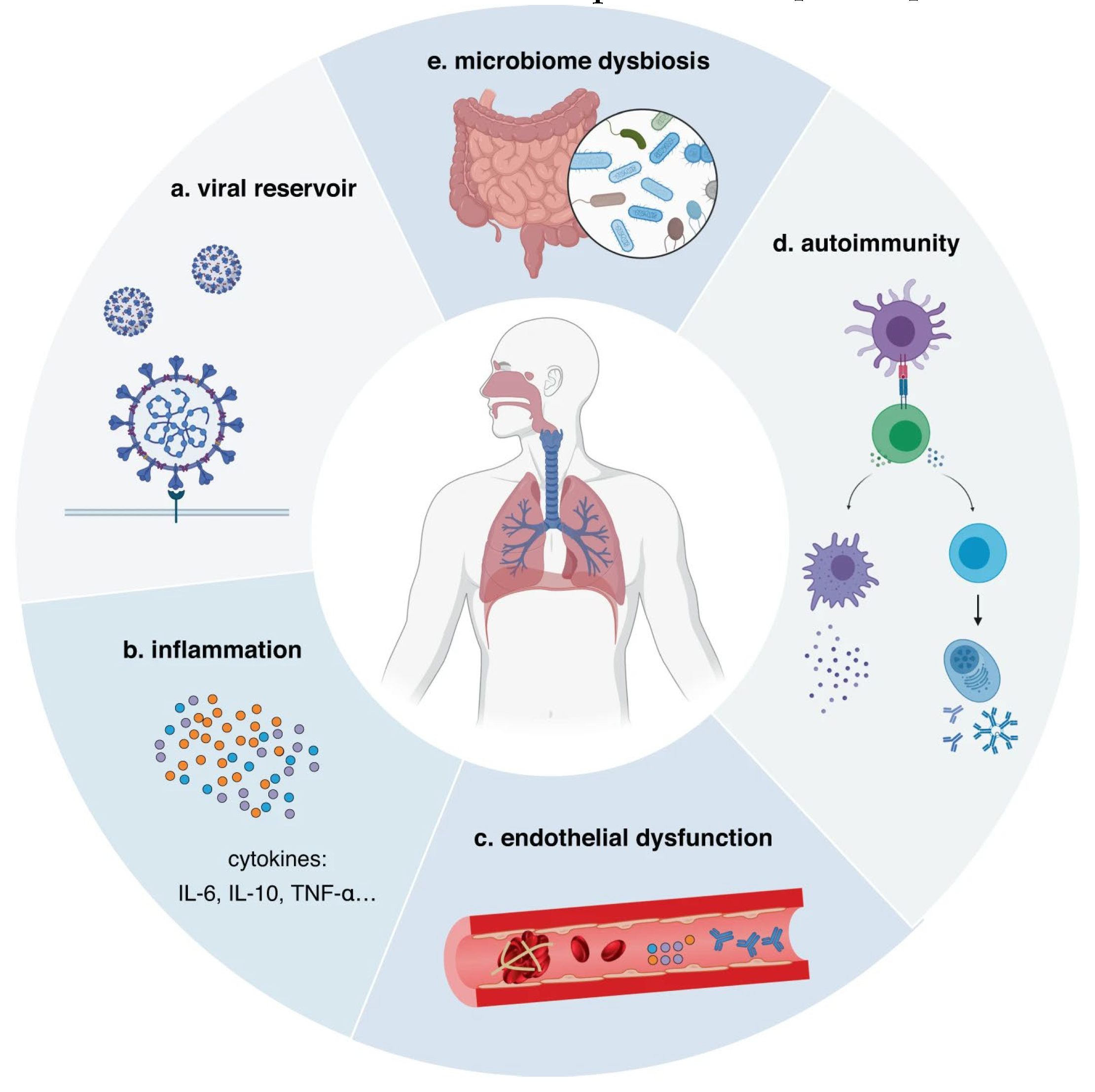
3.2.2. Physiological Mechanisms of Long COVID Formation
3.3. The Social Economic Impact of Long COVID
3.3.1. The Impact of Long COVID on Society
3.3.2. Long COVID's Impact on the Economy
3.3.3. New Clinical Disorders and Accelerated Disease Progression
3.4. Reponses of Major Countries to Long COVID
3.4.1. Reducing the Impact of Long COVID on the Workforce through Policy Adjustments
3.4.2. By Offering Government Fundings to Support Foundational Research on Long COVID
3.4.3. Conducting Investigation to Develop Effective Treatment Strategies for Long COVID
3.4.4. Conducting Development of Vaccines in Prevention and Protection against Long COVID
4. Future Adaptive Management Suggestions and Directions
5. Limitation
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Available online: https://covid19.who.int/ (accessed on 16, March, 2023).
- Logue, J.K.; Franko, N.M.; McCulloch, D.J.; McDonald, D.; Magedson, A.; Wolf, C.R.; Chu, H.Y. Sequelae in adults at 6 months after COVID-19 infection. JAMA network open 2021, 4, e210830–e210830. [Google Scholar] [CrossRef] [PubMed]
- Trihandini, I.; Muhtar, M. The effect of long-haul COVID-19 toward domains of the health-related quality of life among recovered hospitalized patients. Frontiers in Public Health 2023, 11, 1068127. [Google Scholar] [CrossRef] [PubMed]
- Davis, H.E.; McCorkell, L.; Vogel, J.M.; Topol, E.J. Long COVID: major findings, mechanisms and recommendations. Nature Reviews Microbiology 2023, 21, 133–146. [Google Scholar] [CrossRef] [PubMed]
- Iwasaki, A.; Putrino, D. Why we need a deeper understanding of the pathophysiology of long COVID. The Lancet Infectious Diseases 2023, 23, 393–395. [Google Scholar] [CrossRef] [PubMed]
- Natarajan, A.; Shetty, A.; Delanerolle, G.; Zeng, Y.; Zhang, Y.; Raymont, V.; Rathod, S.; Halabi, S.; Elliot, K.; Shi, J.Q. A systematic review and meta-analysis of long COVID symptoms. Systematic reviews 2023, 12, 88. [Google Scholar] [CrossRef] [PubMed]
- Bowyer, R.C.; Huggins, C.; Toms, R.; Shaw, R.J.; Hou, B.; Thompson, E.J.; Kwong, A.S.; Williams, D.M.; Kibble, M.; Ploubidis, G.B. Characterising patterns of COVID-19 and long COVID symptoms: evidence from nine UK longitudinal studies. European journal of epidemiology 2023, 38, 199–210. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; Haupert, S.R.; Zimmermann, L.; Shi, X.; Fritsche, L.G.; Mukherjee, B. Global Prevalence of Post-Coronavirus Disease 2019 (COVID-19) Condition or Long COVID: A Meta-Analysis and Systematic Review. J. Infect. Dis. 2022, 226, 1593–1607. [Google Scholar] [CrossRef] [PubMed]
- Imoto, W.; Yamada, K.; Kawai, R.; Imai, T.; Kawamoto, K.; Uji, M.; Kanda, H.; Takada, M.; Ohno, Y.; Ohtani, H.; et al. A cross-sectional, multicenter survey of the prevalence and risk factors for Long COVID. Sci Rep 2022, 12, 22413. [Google Scholar] [CrossRef] [PubMed]
- Damant, R.W.; Rourke, L.; Cui, Y.; Lam, G.Y.; Smith, M.P.; Fuhr, D.P.; Tay, J.K.; Varughese, R.A.; Laratta, C.R.; Lau, A.; et al. Reliability and validity of the post COVID-19 condition stigma questionnaire: A prospective cohort study. EClinicalMedicine 2023, 55, 101755. [Google Scholar] [CrossRef]
- Mizrahi, B.; Sudry, T.; Flaks-Manov, N.; Yehezkelli, Y.; Kalkstein, N.; Akiva, P.; Ekka-Zohar, A.; Ben David, S.S.; Lerner, U.; Bivas-Benita, M.; et al. Long covid outcomes at one year after mild SARS-CoV-2 infection: nationwide cohort study. BMJ 2023, 380, e072529. [Google Scholar] [CrossRef]
- Wang, S.; Li, Y.; Yue, Y.; Yuan, C.; Kang, J.H.; Chavarro, J.E.; Bhupathiraju, S.N.; Roberts, A.L. Adherence to Healthy Lifestyle Prior to Infection and Risk of Post-COVID-19 Condition. JAMA Intern Med 2023, 183, 232–241. [Google Scholar] [CrossRef] [PubMed]
- Marra, A.R.; Sampaio, V.S.; Ozahata, M.C.; Lopes, R.; Brito, A.F.; Bragatte, M.; Kalil, J.; Miraglia, J.L.; Malheiro, D.T.; Guozhang, Y.; et al. Risk factors for long coronavirus disease 2019 (long COVID) among healthcare personnel, Brazil, 2020-2022. Infect. Control Hosp. Epidemiol. 2023, 1–7. [Google Scholar] [CrossRef]
- Davis, H.E.; Assaf, G.S.; McCorkell, L.; Wei, H.; Low, R.J.; Re'em, Y.; Redfield, S.; Austin, J.P.; Akrami, A. Characterizing long COVID in an international cohort: 7 months of symptoms and their impact. EClinicalMedicine 2021, 38, 101019. [Google Scholar] [CrossRef]
- Iqbal, A.; Iqbal, K.; Ali, S.A.; Azim, D.; Farid, E.; Baig, M.D.; Arif, T.B.; Raza, M. The COVID-19 sequelae: a cross-sectional evaluation of post-recovery symptoms and the need for rehabilitation of COVID-19 survivors. Cureus 2021, 13. [Google Scholar] [CrossRef]
- Mandal, S.; Barnett, J.; Brill, S.E.; Brown, J.S.; Denneny, E.K.; Hare, S.S.; Heightman, M.; Hillman, T.E.; Jacob, J.; Jarvis, H.C. ‘Long-COVID’: a cross-sectional study of persisting symptoms, biomarker and imaging abnormalities following hospitalisation for COVID-19. Thorax 2021, 76, 396–398. [Google Scholar] [CrossRef]
- Gutierrez-Martinez, L.; Karten, J.; Kritzer, M.D.; Josephy-Hernandez, S.; Kim, D.; Newhouse, A.; Pasinski, M.; Praschan, N.; Razafsha, M.; Rubin, D.B.; et al. Post-Acute Sequelae of SARS-CoV-2 Infection: A Descriptive Clinical Study. J. Neuropsychiatry Clin. Neurosci. 2022, 34, 393–405. [Google Scholar] [CrossRef]
- Mallick, D.; Goyal, L.; Chourasia, P.; Zapata, M.R.; Yashi, K.; Surani, S. COVID-19 induced postural orthostatic tachycardia syndrome (POTS): a review. Cureus 2023, 15. [Google Scholar] [CrossRef] [PubMed]
- Reis Carneiro, D.; Rocha, I.; Habek, M.; Helbok, R.; Sellner, J.; Struhal, W.; Wenning, G.; Fanciulli, A. Clinical presentation and management strategies of cardiovascular autonomic dysfunction following a COVID-19 infection–A systematic review. European journal of neurology 2023, 30, 1528–1539. [Google Scholar] [CrossRef] [PubMed]
- Landry, M.; Bornstein, S.; Nagaraj, N.; Sardon, G.A., Jr.; Castel, A.; Vyas, A.; McDonnell, K.; Agneshwar, M.; Wilkinson, A.; Goldman, L. Postacute Sequelae of SARS-CoV-2 in University Setting. Emerg. Infect. Dis. 2023, 29, 519–527. [Google Scholar] [CrossRef]
- Dennis, A.; Cuthbertson, D.J.; Wootton, D.; Crooks, M.; Gabbay, M.; Eichert, N.; Mouchti, S.; Pansini, M.; Roca-Fernandez, A.; Thomaides-Brears, H.; et al. Multi-organ impairment and long COVID: a 1-year prospective, longitudinal cohort study. J. R. Soc. Med. 2023, 116, 97–112. [Google Scholar] [CrossRef]
- Baskett, W.I.; Qureshi, A.I.; Shyu, D.; Armer, J.M.; Shyu, C.-R. COVID-Specific Long-term Sequelae in Comparison to Common Viral Respiratory Infections: An Analysis of 17 487 Infected Adult Patients. Open Forum Infectious Diseases 2022, 10. [Google Scholar] [CrossRef] [PubMed]
- Jia, X.; Cao, S.; Lee, A.S.; Manohar, M.; Sindher, S.B.; Ahuja, N.; Artandi, M.; Blish, C.A.; Blomkalns, A.L.; Chang, I.; et al. Anti-nucleocapsid antibody levels and pulmonary comorbid conditions are linked to post-COVID-19 syndrome. JCI Insight 2022, 7, e156713. [Google Scholar] [CrossRef]
- Matta, J.; Wiernik, E.; Robineau, O.; Carrat, F.; Touvier, M.; Severi, G.; de Lamballerie, X.; Blanché, H.; Deleuze, J.-F.; Gouraud, C. Association of self-reported COVID-19 infection and SARS-CoV-2 serology test results with persistent physical symptoms among French adults during the COVID-19 pandemic. JAMA internal medicine 2022, 182, 19–25. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Pérez, O.; Merino, E.; Leon-Ramirez, J.-M.; Andres, M.; Ramos, J.M.; Arenas-Jiménez, J.; Asensio, S.; Sanchez, R.; Ruiz-Torregrosa, P.; Galan, I. Post-acute COVID-19 syndrome. Incidence and risk factors: A Mediterranean cohort study. Journal of Infection 2021, 82, 378–383. [Google Scholar]
- Augustin, M.; Schommers, P.; Stecher, M.; Dewald, F.; Gieselmann, L.; Gruell, H.; Horn, C.; Vanshylla, K.; Di Cristanziano, V.; Osebold, L. Post-COVID syndrome in non-hospitalised patients with COVID-19: a longitudinal prospective cohort study. The Lancet Regional Health–Europe 2021, 6.
- Cabrera Martimbianco, A.L.; Pacheco, R.L.; Bagattini, Â.M.; Riera, R. Frequency, signs and symptoms, and criteria adopted for long COVID-19: A systematic review. International journal of clinical practice 2021, 75, e14357. [Google Scholar] [CrossRef]
- Nabavi, N. Long covid: How to define it and how to manage it. BMJ 2020, 370, m3489. [Google Scholar] [CrossRef]
- Available online: https://www.umu.se/en/news/research-to-spread-light-on-long-covid-uncertainties_11713455/ (accessed on 2023-01-26).
- Song, Z.; Giuriato, M. Demographic And Clinical Factors Associated With Long COVID. Health Aff. (Millwood) 2023, 42, 433–442. [Google Scholar] [CrossRef] [PubMed]
- Herman, J.D.; Atyeo, C.; Zur, Y.; Cook, C.E.; Patel, N.J.; Vanni, K.M.; Kowalski, E.N.; Qian, G.; Srivatsan, S.; Shadick, N.A.; et al. Humoral immunity to an endemic coronavirus is associated with postacute sequelae of COVID-19 in individuals with rheumatic diseases. Sci. Transl. Med. 2023, 15, eadf6598. [Google Scholar] [CrossRef] [PubMed]
- Gil, S.; de Oliveira Júnior, G.N.; Sarti, F.M.; Filho, W.J.; Longobardi, I.; Turri, J.A.O.; Shinjo, S.K.; Ferriolli, E.; Avelino-Silva, T.J.; Busse, A.L.; et al. Acute Muscle Mass Loss Predicts Long-Term Fatigue, Myalgia, and Health Care Costs in COVID-19 Survivors. Journal of the American Medical Directors Association 2023, 24, 10–16. [Google Scholar] [CrossRef]
- Wang, S.; Quan, L.; Chavarro, J.E.; Slopen, N.; Kubzansky, L.D.; Koenen, K.C.; Kang, J.H.; Weisskopf, M.G.; Branch-Elliman, W.; Roberts, A.L. Associations of Depression, Anxiety, Worry, Perceived Stress, and Loneliness Prior to Infection With Risk of Post-COVID-19 Conditions. JAMA Psychiatry 2022, 79, 1081–1091. [Google Scholar] [CrossRef]
- Fischer, A.; Zhang, L.; Elbeji, A.; Wilmes, P.; Oustric, P.; Staub, T.; Nazarov, P.V.; Ollert, M.; Fagherazzi, G. Long COVID Symptomatology After 12 Months and Its Impact on Quality of Life According to Initial Coronavirus Disease 2019 Disease Severity. Open Forum Infect Dis 2022, 9, ofac397. [Google Scholar] [CrossRef] [PubMed]
- Klein, J.; Wood, J.; Jaycox, J.; Dhodapkar, R.M.; Lu, P.; Gehlhausen, J.R.; Tabachnikova, A.; Greene, K.; Tabacof, L.; Malik, A.A.; et al. Distinguishing features of Long COVID identified through immune profiling. Nature 2023.
- Hopkins, F.R.; Govender, M.; Svanberg, C.; Nordgren, J.; Waller, H.; Nilsdotter-Augustinsson, A.; Henningsson, A.J.; Hagbom, M.; Sjowall, J.; Nystrom, S.; et al. Major alterations to monocyte and dendritic cell subsets lasting more than 6 months after hospitalization for COVID-19. Front Immunol 2022, 13, 1082912. [Google Scholar] [CrossRef] [PubMed]
- Littlefield, K.M.; Watson, R.O.; Schneider, J.M.; Neff, C.P.; Yamada, E.; Zhang, M.; Campbell, T.B.; Falta, M.T.; Jolley, S.E.; Fontenot, A.P.; et al. SARS-CoV-2-specific T cells associate with inflammation and reduced lung function in pulmonary post-acute sequalae of SARS-CoV-2. PLoS Pathog. 2022, 18, e1010359. [Google Scholar] [CrossRef] [PubMed]
- Wisk, L.E.; Gottlieb, M.A.; Spatz, E.S.; Yu, H.; Wang, R.C.; Slovis, B.H.; Saydah, S.; Plumb, I.D.; O'Laughlin, K.N.; Montoy, J.C.C.; et al. Association of Initial SARS-CoV-2 Test Positivity With Patient-Reported Well-being 3 Months After a Symptomatic Illness. JAMA Netw Open 2022, 5, e2244486. [Google Scholar] [CrossRef] [PubMed]
- Astin, R.; Banerjee, A.; Baker, M.R.; Dani, M.; Ford, E.; Hull, J.H.; Lim, P.B.; McNarry, M.; Morten, K.; O'Sullivan, O.; et al. Long COVID: mechanisms, risk factors and recovery. Exp. Physiol. 2023, 108, 12–27. [Google Scholar] [CrossRef] [PubMed]
- Badran, B.W.; Huffman, S.M.; Dancy, M.; Austelle, C.W.; Bikson, M.; Kautz, S.A.; George, M.S. A pilot randomized controlled trial of supervised, at-home, self-administered transcutaneous auricular vagus nerve stimulation (taVNS) to manage long COVID symptoms. Res Sq 2022. [CrossRef]
- Badran, B.W.; Huffman, S.M.; Dancy, M.; Austelle, C.W.; Bikson, M.; Kautz, S.A.; George, M.S. A pilot randomized controlled trial of supervised, at-home, self-administered transcutaneous auricular vagus nerve stimulation (taVNS) to manage long COVID symptoms. Bioelectron Med 2022, 8, 13. [Google Scholar] [CrossRef] [PubMed]
- Colzato, L.S.; Elmers, J.; Beste, C.; Hommel, B. A Prospect to Ameliorate Affective Symptoms and to Enhance Cognition in Long COVID Using Auricular Transcutaneous Vagus Nerve Stimulation. J Clin Med 2023, 12. [Google Scholar] [CrossRef]
- Oaklander, A.L.; Mills, A.J.; Kelley, M.; Toran, L.S.; Smith, B.; Dalakas, M.C.; Nath, A. Peripheral Neuropathy Evaluations of Patients With Prolonged Long COVID. Neurol Neuroimmunol Neuroinflamm 2022, 9. [Google Scholar] [CrossRef]
- Klein, J.; Wood, J.; Jaycox, J.; Dhodapkar, R.M.; Lu, P.; Gehlhausen, J.R.; Tabachnikova, A.; Greene, K.; Tabacof, L.; Malik, A.A.; et al. Distinguishing features of Long COVID identified through immune profiling. Nature 2023. [CrossRef] [PubMed]
- Kubankova, M.; Hohberger, B.; Hoffmanns, J.; Furst, J.; Herrmann, M.; Guck, J.; Krater, M. Physical phenotype of blood cells is altered in COVID-19. Biophys. J. 2021, 120, 2838–2847. [Google Scholar] [CrossRef] [PubMed]
- Cervia-Hasler, C.; Brüningk, S.C.; Hoch, T.; Fan, B.; Muzio, G.; Thompson, R.C.; Ceglarek, L.; Meledin, R.; Westermann, P.; Emmenegger, M.; et al. Persistent complement dysregulation with signs of thromboinflammation in active Long Covid. Science 2024, 383, eadg7942. [Google Scholar] [CrossRef] [PubMed]
- Greene, C.; Connolly, R.; Brennan, D.; Laffan, A.; O’Keeffe, E.; Zaporojan, L.; O’Callaghan, J.; Thomson, B.; Connolly, E.; Argue, R.; et al. Blood–brain barrier disruption and sustained systemic inflammation in individuals with long COVID-associated cognitive impairment. Nature Neuroscience 2024. [CrossRef] [PubMed]
- Saladino, V.; Algeri, D.; Auriemma, V. The psychological and social impact of Covid-19: new perspectives of well-being. Frontiers in psychology 2020, 11, 577684. [Google Scholar] [CrossRef] [PubMed]
- Ali, I.; Alharbi, O.M. COVID-19: Disease, management, treatment, and social impact. Science of the total Environment 2020, 728, 138861. [Google Scholar] [CrossRef] [PubMed]
- Long, E.; Patterson, S.; Maxwell, K.; Blake, C.; Pérez, R.B.; Lewis, R.; McCann, M.; Riddell, J.; Skivington, K.; Wilson-Lowe, R. COVID-19 pandemic and its impact on social relationships and health. J Epidemiol Community Health 2022, 76, 128–132. [Google Scholar] [CrossRef] [PubMed]
- Evans, R.A.; McAuley, H.; Harrison, E.M.; Shikotra, A.; Singapuri, A.; Sereno, M.; Elneima, O.; Docherty, A.B.; Lone, N.I.; Leavy, O.C.; et al. Physical, cognitive, and mental health impacts of COVID-19 after hospitalisation (PHOSP-COVID): a UK multicentre, prospective cohort study. Lancet Respir Med 2021, 9, 1275–1287. [Google Scholar] [CrossRef]
- Van Wambeke, E.; Bezler, C.; Kasprowicz, A.M.; Charles, A.L.; Andres, E.; Geny, B. Two-Years Follow-Up of Symptoms and Return to Work in Complex Post-COVID-19 Patients. J Clin Med 2023, 12. [Google Scholar] [CrossRef]
- Aburto, J.M.; Scholey, J.; Kashnitsky, I.; Zhang, L.; Rahal, C.; Missov, T.I.; Mills, M.C.; Dowd, J.B.; Kashyap, R. Quantifying impacts of the COVID-19 pandemic through life-expectancy losses: a population-level study of 29 countries. Int. J. Epidemiol. 2022, 51, 63–74. [Google Scholar] [CrossRef]
- Hampshire, A.; Chatfield, D.A.; Mphil, A.M.; Jolly, A.; Trender, W.; Hellyer, P.J.; Giovane, M.D.; Newcombe, V.F.J.; Outtrim, J.G.; Warne, B.; et al. Multivariate profile and acute-phase correlates of cognitive deficits in a COVID-19 hospitalised cohort. eClinicalMedicine 2022, 47. [Google Scholar] [CrossRef]
- Zhao, Y.; Shi, L.; Jiang, Z.; Zeng, N.; Mei, H.; Lu, Y.; Yang, J.; Jin, F.; Ni, S.; Wu, S.; et al. The phenotype and prediction of long-term physical, mental and cognitive COVID-19 sequelae 20 months after recovery, a community-based cohort study in China. Mol. Psychiatry 2023, 28, 1793–1801. [Google Scholar] [CrossRef] [PubMed]
- Suran, M. Long COVID Linked With Unemployment in New Analysis. JAMA 2023, 329, 701–702. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.weforum.org/agenda/2022/08/long-covid-work-economy-united-states-health (accessed on Aug 30, 2022).
- Available online: https://www.bankofengland.co.uk/speech/2022/may/michael-saunders-speech-at-the-resolution-foundation-event (accessed on 09 May 2022).
- Available online: https://www.hhs.gov/civil-rights/for-providers/civil-rights-covid19/guidance-long-covid-disability/index.html#footnote3_25o93ze (accessed on July 26, 2021).
- Hussain, Z.; Rizvi, L.J.; Sheikh, H. The Equality Act (2010)-pre-and post-pandemic historic development on equality and discrimination issues for employers: review of literature. International Journal of Law and Management 2022, 64, 168–183. [Google Scholar] [CrossRef]
- Available online: https://www.sydney.edu.au/news-opinion/news/2022/06/30/long-covid-presents-a-major-health-challenge-how-can-australia-b.html (accessed on 30 June 2022).
- Available online: https://www.pennmedicine.org/for-health-care-professionals/for-physicians/covid-information/post-covid19-assessment-and-recovery-clinic-at-penn (accessed on.
- Available online: http://news.china.com.cn/2023-01/13/content_85058563.html (accessed on 2023-01-13).
- Available online: https://www.canada.ca/en/public-health/news/2022/12/government-of-canada-welcomes-task-force-report-on-post-covid-19-condition.html (accessed on December 14, 2022).
- Gandjour, A. Long COVID: Costs for the German economy and health care and pension system. BMC Health Services Research 2023, 23, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.ukri.org/news/18-5-million-to-tackle-long-covid-in-the-community/ (accessed on 18 February 2021).
- Available online: https://www.ukri.org/news/uk-japanese-collaboration-to-address-covid-19-challenges/ (accessed on 30 March 2022).
- Lu, J.Y.; Wilson, J.; Hou, W.; Fleysher, R.; Herold, B.C.; Herold, K.C.; Duong, T.Q. Incidence of new-onset in-hospital and persistent diabetes in COVID-19 patients: comparison with influenza. EBioMedicine 2023, 90, 104487. [Google Scholar] [CrossRef]
- Xu, A.Y.; Wang, S.H.; Duong, T.Q. Patients with prediabetes are at greater risk of developing diabetes 5 months postacute SARS-CoV-2 infection: a retrospective cohort study. BMJ Open Diabetes Res Care 2023, 11, e003257. [Google Scholar] [CrossRef]
- Xie, Y.; Al-Aly, Z. Risks and burdens of incident diabetes in long COVID: a cohort study. Lancet Diabetes Endocrinol 2022. [CrossRef]
- Zhang, V.; Fisher, M.; Hou, W.; Zhang, L.; Duong, T.Q. Incidence of New-Onset Hypertension Post-COVID-19: Comparison With Influenza. Hypertension 2023, 80, 2135–2148. [Google Scholar] [CrossRef] [PubMed]
- Lu, J.Y.; Boparai, M.S.; Shi, C.; Henninger, E.M.; Rangareddy, M.; Veeraraghavan, S.; Mirhaji, P.; Fisher, M.C.; Duong, T.Q. Long-term outcomes of COVID-19 survivors with hospital AKI: association with time to recovery from AKI. Nephrol Dial Transplant 2023. [CrossRef]
- Zhang, Y.; Zhao, Y.; Wang, J.; Zheng, X.; Xu, D.; Lv, J.; Yang, L. Long-term renal outcomes of patients with COVID-19: a meta-analysis of observational studies. J Nephrol 2023, 36, 2441–2456. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Zhou, X.; Chen, Y.; Wang, L.; Zhu, B.; Jiang, Y.; Bu, P.; Liu, W.; Li, D.; Li, Y.; et al. Changes in Home Blood Pressure Monitored Among Elderly Patients With Hypertension During the COVID-19 Outbreak: A Longitudinal Study in China Leveraging a Smartphone-Based Application. Circ Cardiovasc Qual Outcomes 2021, 14, e007098. [Google Scholar] [CrossRef] [PubMed]
- Gotanda, H.; Liyanage-Don, N.; Moran, A.E.; Krousel-Wood, M.; Green, J.B.; Zhang, Y.; Nuckols, T.K. Changes in Blood Pressure Outcomes Among Hypertensive Individuals During the COVID-19 Pandemic: A Time Series Analysis in Three US Healthcare Organizations. Hypertension 2022, 79, 2733–2742. [Google Scholar] [CrossRef]
- Bouwmans, P.; Malahe, S.R.K.; Messchendorp, A.L.; Vart, P.; Imhof, C.; Sanders, J.F.; Gansevoort, R.T.; de Vries, A.P.J.; Abrahams, A.C.; Bemelman, F.J.; et al. Post COVID-19 condition imposes significant burden in patients with advanced chronic kidney disease: A nested case-control study. Int J Infect Dis 2024, 142, 106990. [Google Scholar] [CrossRef] [PubMed]
- Etemadifar, M.; Abhari, A.P.; Nouri, H.; Salari, M.; Maleki, S.; Amin, A.; Sedaghat, N. Does COVID-19 increase the long-term relapsing-remitting multiple sclerosis clinical activity? A cohort study. BMC Neurol 2022, 22, 64. [Google Scholar] [CrossRef] [PubMed]
- Etemadifar, M.; Sedaghat, N.; Aghababaee, A.; Kargaran, P.K.; Maracy, M.R.; Ganjalikhani-Hakemi, M.; Rayani, M.; Abhari, A.P.; Khorvash, R.; Salari, M.; et al. COVID-19 and the Risk of Relapse in Multiple Sclerosis Patients: A Fight with No Bystander Effect? Mult Scler Relat Disord 2021, 51, 102915. [Google Scholar] [CrossRef] [PubMed]
- Montini, F.; Nozzolillo, A.; Tedone, N.; Mistri, D.; Rancoita, P.M.; Zanetta, C.; Mandelli, A.; Furlan, R.; Moiola, L.; Martinelli, V.; et al. COVID-19 has no impact on disease activity, progression and cognitive performance in people with multiple sclerosis: a 2-year study. J Neurol Neurosurg Psychiatry 2023. [CrossRef]
- Andersen, M.L.; Zegers, F.D.; Jolving, L.R.; Knudsen, T.; Stenager, E.; Norgard, B.M. Patients with multiple sclerosis: COVID-19 related disease activity and hospitalisations based on a nationwide cohort study. Mult Scler Relat Disord 2023, 79, 105031. [Google Scholar] [CrossRef] [PubMed]
- Conway, S.E.; Healy, B.C.; Zurawski, J.; Severson, C.; Kaplan, T.; Stazzone, L.; Galetta, K.; Chitnis, T.; Houtchens, M.K. COVID-19 severity is associated with worsened neurological outcomes in multiple sclerosis and related disorders. Mult Scler Relat Disord 2022, 63, 103946. [Google Scholar] [CrossRef]
- Hadidchi, R.; Wang, S.H.; Rezko, D.; Henry, S.; Coyle, P.K.; Duong, T.Q. SARS-CoV-2 infection increases long-term multiple sclerosis disease activity and all-cause mortality in an underserved inner-city population. Mult Scler Relat Disord 2024, 86, 105613. [Google Scholar] [CrossRef]
- Brown, E.E.; Kumar, S.; Rajji, T.K.; Pollock, B.G.; Mulsant, B.H. Anticipating and Mitigating the Impact of the COVID-19 Pandemic on Alzheimer's Disease and Related Dementias. Am J Geriatr Psychiatry 2020, 28, 712–721. [Google Scholar] [CrossRef] [PubMed]
- Coolen, T.; Lolli, V.; Sadeghi, N.; Rovai, A.; Trotta, N.; Taccone, F.S.; Creteur, J.; Henrard, S.; Goffard, J.C.; Dewitte, O.; et al. Early postmortem brain MRI findings in COVID-19 non-survivors. Neurology 2020, 95, e2016–e2027. [Google Scholar] [CrossRef] [PubMed]
- Boruah, A.P.; Thakur, K.T.; Gadani, S.P.; Kothari, K.U.; Chomba, M.; Guekht, A.; Heydari, K.; Hoo, F.K.; Hwang, S.; Michael, B.D.; et al. Pre-existing neurological conditions and COVID-19 co-infection: Data from systematic reviews, meta-analyses, and scoping reviews. J Neurol Sci 2023, 455, 120858. [Google Scholar] [CrossRef] [PubMed]
- Eligulashvili, A.; Gordon, M.; Lee, J.S.; Lee, J.; Mehrotra-Varma, S.; Mehrotra-Varma, J.; Hsu, K.; Hilliard, I.; Lee, K.; Li, A.; et al. Long-term outcomes of hospitalized patients with SARS-CoV-2/COVID-19 with and without neurological involvement: 3-year follow-up assessment. PLoS Med 2024, 21, e1004263. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Qian, J.; Wang, Y.; Wang, J.; Mi, X.; Qu, L.; Song, N.; Xie, J. Potential convergence of olfactory dysfunction in Parkinson's disease and COVID-19: The role of neuroinflammation. Ageing Res Rev 2024, 97, 102288. [Google Scholar] [CrossRef] [PubMed]
- Bougea, A.; Georgakopoulou, V.E.; Palkopoulou, M.; Efthymiopoulou, E.; Angelopoulou, E.; Spandidos, D.A.; Zikos, P. New-onset non-motor symptoms in patients with Parkinson's disease and post-COVID-19 syndrome: A prospective cross-sectional study. Med Int (Lond) 2023, 3, 23. [Google Scholar] [CrossRef] [PubMed]
- Weiss, M.; Gutzeit, J.; Appel, K.S.; Bahmer, T.; Beutel, M.; Deckert, J.; Fricke, J.; Hanss, S.; Hettich-Damm, N.; Heuschmann, P.U.; et al. Depression and fatigue six months post-COVID-19 disease are associated with overlapping symptom constellations: A prospective, multi-center, population-based cohort study. J Affect Disord 2024, 352, 296–305. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://news.cuanschutz.edu/cctsi/nationwide-study-of-long-covid-to-launch-at-university-of-colorado-anschutz-medical-campus (accessed on February 7, 2022).
- National Research Action Plan on Long COVID. Available online. (accessed on August 2022).
- Samudyata; Oliveira, A. O.; Malwade, S.; Rufino de Sousa, N.; Goparaju, S.K.; Gracias, J.; Orhan, F.; Steponaviciute, L.; Schalling, M.; Sheridan, S.D.; et al. SARS-CoV-2 promotes microglial synapse elimination in human brain organoids. Mol. Psychiatry 2022, 27, 3939–3950. [CrossRef]
- Adult Stem Cell Therapy for COVID-19 Sequelae Begins in Japan for the First Time in the World.
- Ra, J.C.; Shin, I.S.; Kim, S.H.; Kang, S.K.; Kang, B.C.; Lee, H.Y.; Kim, Y.J.; Jo, J.Y.; Yoon, E.J.; Choi, H.J.; et al. Safety of intravenous infusion of human adipose tissue-derived mesenchymal stem cells in animals and humans. Stem Cells Dev. 2011, 20, 1297–1308. [Google Scholar] [CrossRef] [PubMed]
- Havervall, S.; Marking, U.; Svensson, J.; Greilert-Norin, N.; Bacchus, P.; Nilsson, P.; Hober, S.; Gordon, M.; Blom, K.; Klingstrom, J.; et al. Anti-Spike Mucosal IgA Protection against SARS-CoV-2 Omicron Infection. N. Engl. J. Med. 2022, 387, 1333–1336. [Google Scholar] [CrossRef]
- Yan, C.H.; Jang, S.S.; Lin, H.C.; Ma, Y.; Khanwalkar, A.R.; Thai, A.; Patel, Z.M. Use of platelet-rich plasma for COVID-19-related olfactory loss: a randomized controlled trial. Int Forum Allergy Rhinol 2023, 13, 989–997. [Google Scholar] [CrossRef] [PubMed]
- Satoh, T.; Trudler, D.; Oh, C.K.; Lipton, S.A. Potential Therapeutic Use of the Rosemary Diterpene Carnosic Acid for Alzheimer's Disease, Parkinson's Disease, and Long-COVID through NRF2 Activation to Counteract the NLRP3 Inflammasome. Antioxidants (Basel) 2022, 11. [Google Scholar] [CrossRef] [PubMed]
- Jha, V. Colchicine to Reduce Coronavirus Disease-19 Related Inflammation and Cardiovascular complications in High-Risk Patients Post-Acute Infection With SARS-COV. 2021.
- Could low-dose lithium treat long COVID? UB launches clinical trial to find out. Available online: https://www.buffalo.edu/news/releases/2023/01/002.html (accessed on January 6, 2023).
- Effect of Lithium Therapy on Long COVID Symptoms. Available online: https://www.clinicaltrials.gov/ct2/show/NCT05618587?term=Guttuso&cond=Long+COVID&draw=2&rank=1 (accessed on November 16, 2022).
- Saunders, C.; Sperling, S.; Bendstrup, E. A new paradigm is needed to explain long COVID. Lancet Respir Med 2023, 11, e12–e13. [Google Scholar] [CrossRef] [PubMed]
- Fagherazzi, G.; Zhang, L.; Elbeji, A.; Higa, E.; Despotovic, V.; Ollert, M.; Aguayo, G.A.; Nazarov, P.V.; Fischer, A. A voice-based biomarker for monitoring symptom resolution in adults with COVID-19: Findings from the prospective Predi-COVID cohort study. PLOS Digit Health 2022, 1, e0000112. [Google Scholar] [CrossRef] [PubMed]
- Kovarik, J.J.; Bileck, A.; Hagn, G.; Meier-Menches, S.M.; Frey, T.; Kaempf, A.; Hollenstein, M.; Shoumariyeh, T.; Skos, L.; Reiter, B.; et al. A multi-omics based anti-inflammatory immune signature characterizes long COVID-19 syndrome. iScience 2023, 26, 105717. [Google Scholar] [CrossRef] [PubMed]
- Kuchler, T.; Gunthner, R.; Ribeiro, A.; Hausinger, R.; Streese, L.; Wohnl, A.; Kesseler, V.; Negele, J.; Assali, T.; Carbajo-Lozoya, J.; et al. Persistent endothelial dysfunction in post-COVID-19 syndrome and its associations with symptom severity and chronic inflammation. Angiogenesis 2023, 26, 547–563. [Google Scholar] [CrossRef] [PubMed]
- Krishna, B.A.; Metaxaki, M.; Wills, M.R.; Sithole, N. Reduced Incidence of Long Coronavirus Disease Referrals to the Cambridge University Teaching Hospital Long Coronavirus Disease Clinic. Clin. Infect. Dis. 2023, 76, 738–740. [Google Scholar] [CrossRef] [PubMed]
- Al-Aly, Z.; Bowe, B.; Xie, Y. Long COVID after breakthrough SARS-CoV-2 infection. Nat. Med. 2022, 28, 1461–1467. [Google Scholar] [CrossRef] [PubMed]
- Richard, S.A.; Pollett, S.D.; Fries, A.C.; Berjohn, C.M.; Maves, R.C.; Lalani, T.; Smith, A.G.; Mody, R.M.; Ganesan, A.; Colombo, R.E.; et al. Persistent COVID-19 Symptoms at 6 Months After Onset and the Role of Vaccination Before or After SARS-CoV-2 Infection. JAMA Netw Open 2023, 6, e2251360. [Google Scholar] [CrossRef]
- Palmer, C.D.; Scallan, C.D.; Kraemer Tardif, L.D.; Kachura, M.A.; Rappaport, A.R.; Koralek, D.O.; Uriel, A.; Gitlin, L.; Klein, J.; Davis, M.J.; et al. GRT-R910: a self-amplifying mRNA SARS-CoV-2 vaccine boosts immunity for >/=6 months in previously-vaccinated older adults. Nat. Commun. 2023, 14, 3274. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).