Submitted:
19 February 2026
Posted:
20 February 2026
You are already at the latest version
Abstract
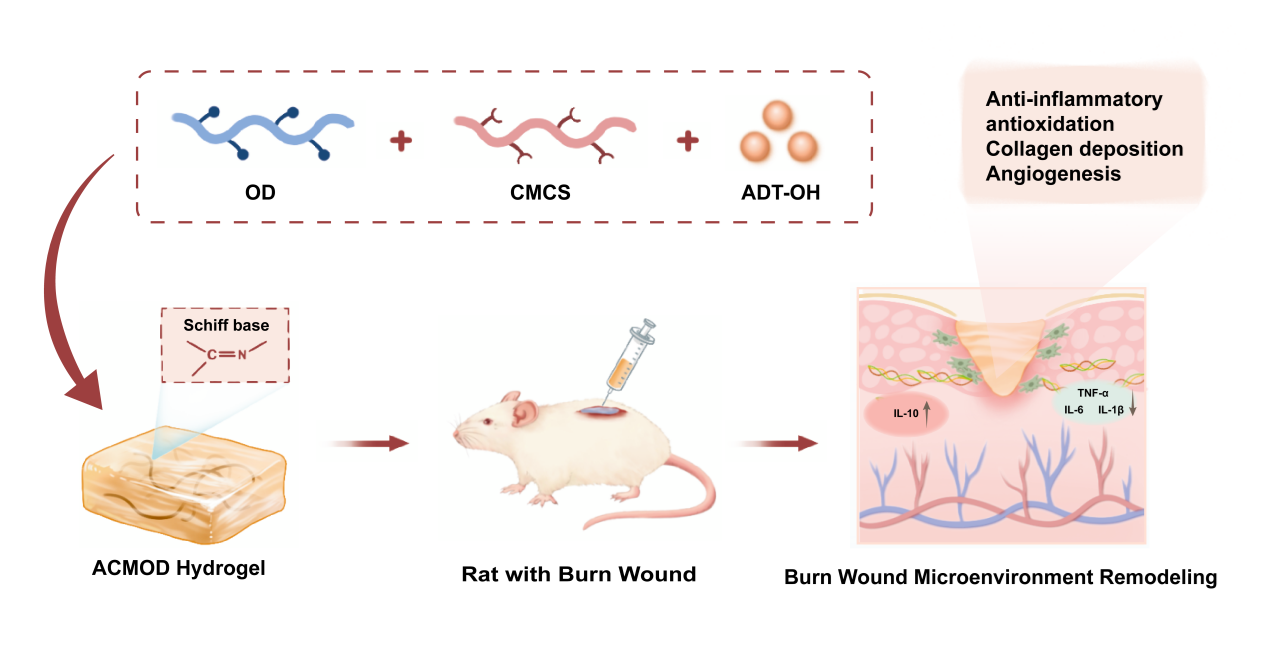
Keywords:
1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Synthesis of Oxidized Dextran
2.3. Characterization of OD
2.4. Preparation of Hydrogels
2.5. Self-Healing Property of the Hydrogel
2.6. Scanning Electron Microscopy (SEM) Analysis
2.7. Rheological Characterization
2.8. Swelling Behavior of the Hydrogel
2.9. In Vitro Drug Release from ACMOD Hydrogel
2.10. H₂S Release from ACMOD Hydrogel
2.11. Hemolysis Assay
2.12. Cell Culture
2.13. Preparation of Hydrogel Extract
2.14. MTT Assay
2.15. Live/Dead Staining
2.16. Cell Scratch Assay
2.17. Transwell Migration Assay
2.18. In Vitro ROS Scavenging Assay
2.19. In Vitro Detection of Intracellular H₂S
2.20. Tube Formation Assay
2.21. In Vivo Study of ACMOD Hydrogel on Burn Wound Healing
2.22. Quantification of Inflammatory Cytokines
2.23. Determination of Oxidative Stress Levels in Wound Tissue
2.24. Immunofluorescence Staining of Macrophage Markers in Wound Tissue
2.25. Immunofluorescence Staining of VEGF in Wound Tissue
2.26. Histological Analysis
2.27. In Vivo Safety Assessment
2.28. Statistical Analysis
3. Results and Discussion
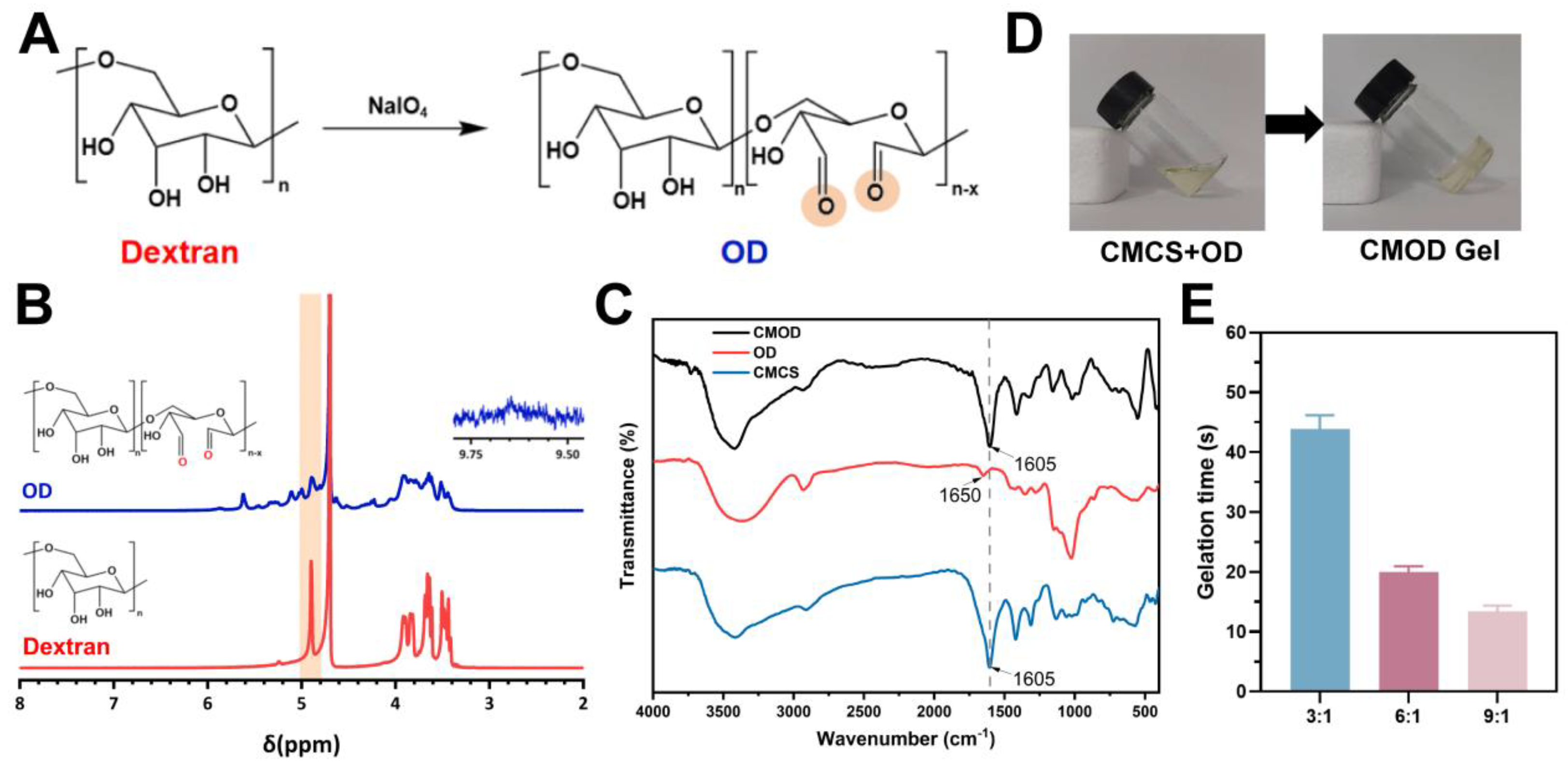
3.1. Synthesis and Characterization of OD and Hydrogels
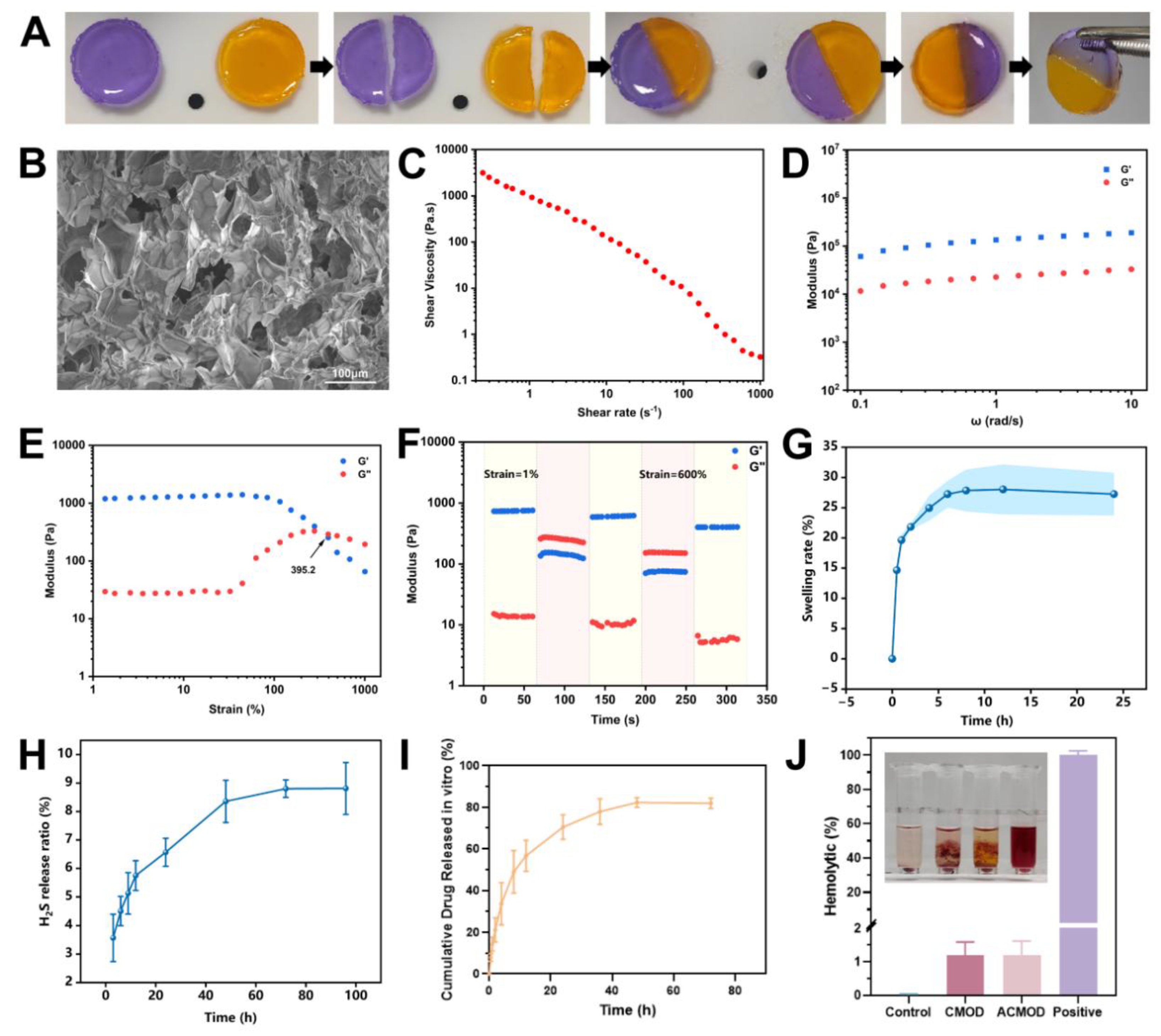
3.2. Morphological and Rheological Properties of the Hydrogel
3.3. Swelling and Hydrogen Sulfide Generation Properties
3.4. In Vitro Drug Release Profile
3.5. Hemocompatibility Assessment
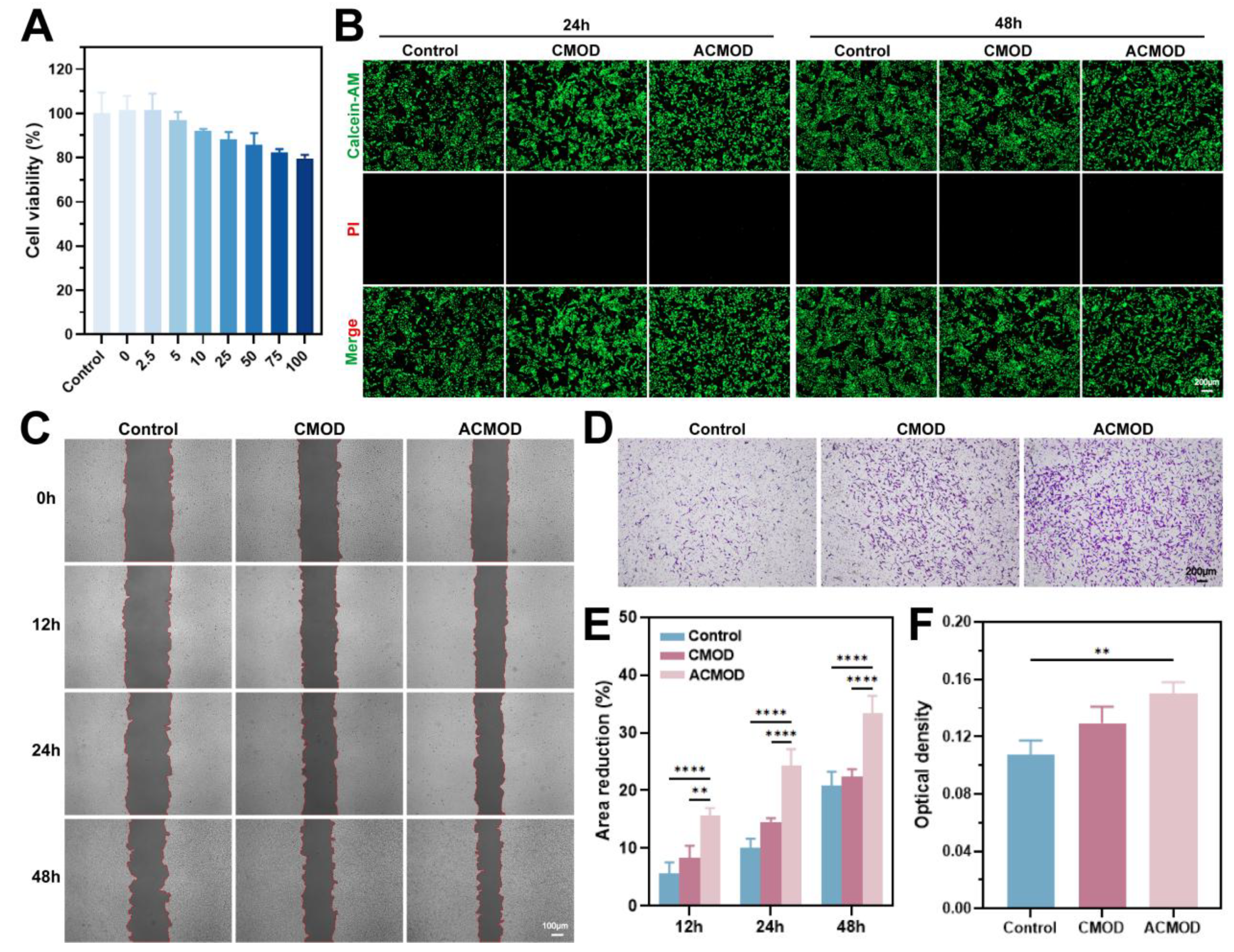
3.6. In Vitro Biocompatibility and Cell Migration Assays
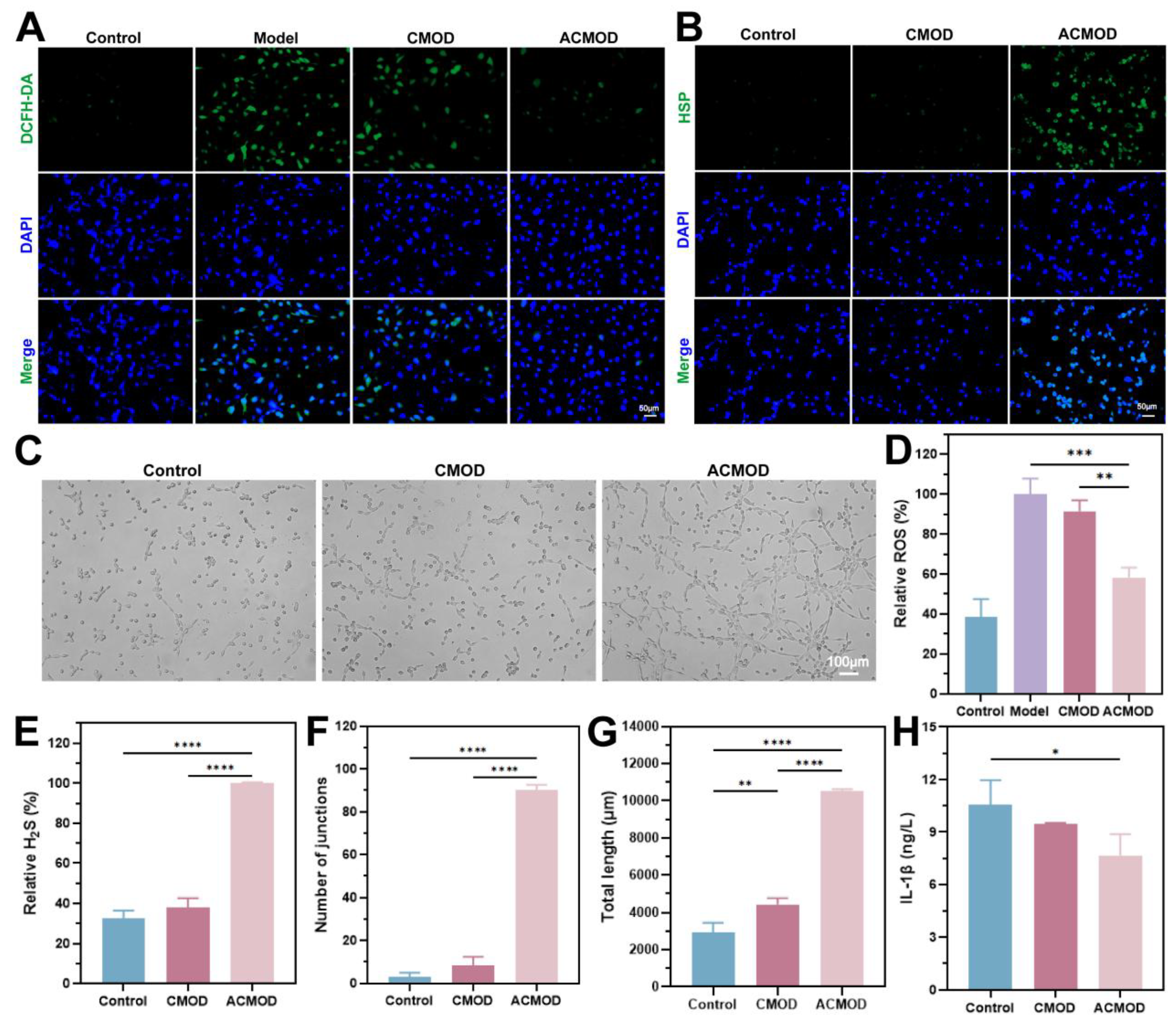
3.7. In Vitro Antioxidant, H₂S-Generating, Pro-Angiogenic and anti-inflammatory Properties
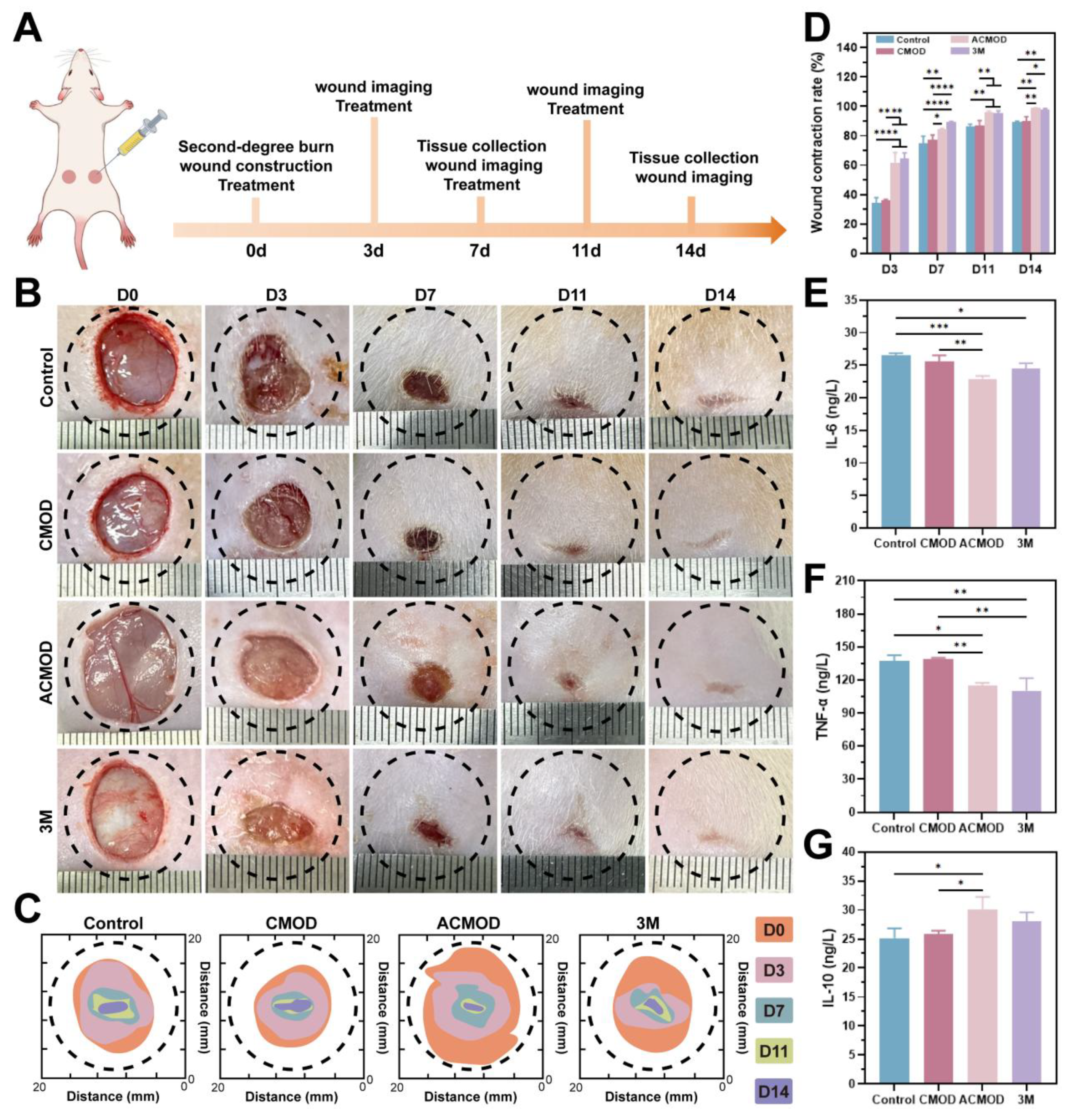
3.8. In Vivo Evaluation of Burn Wound Healing
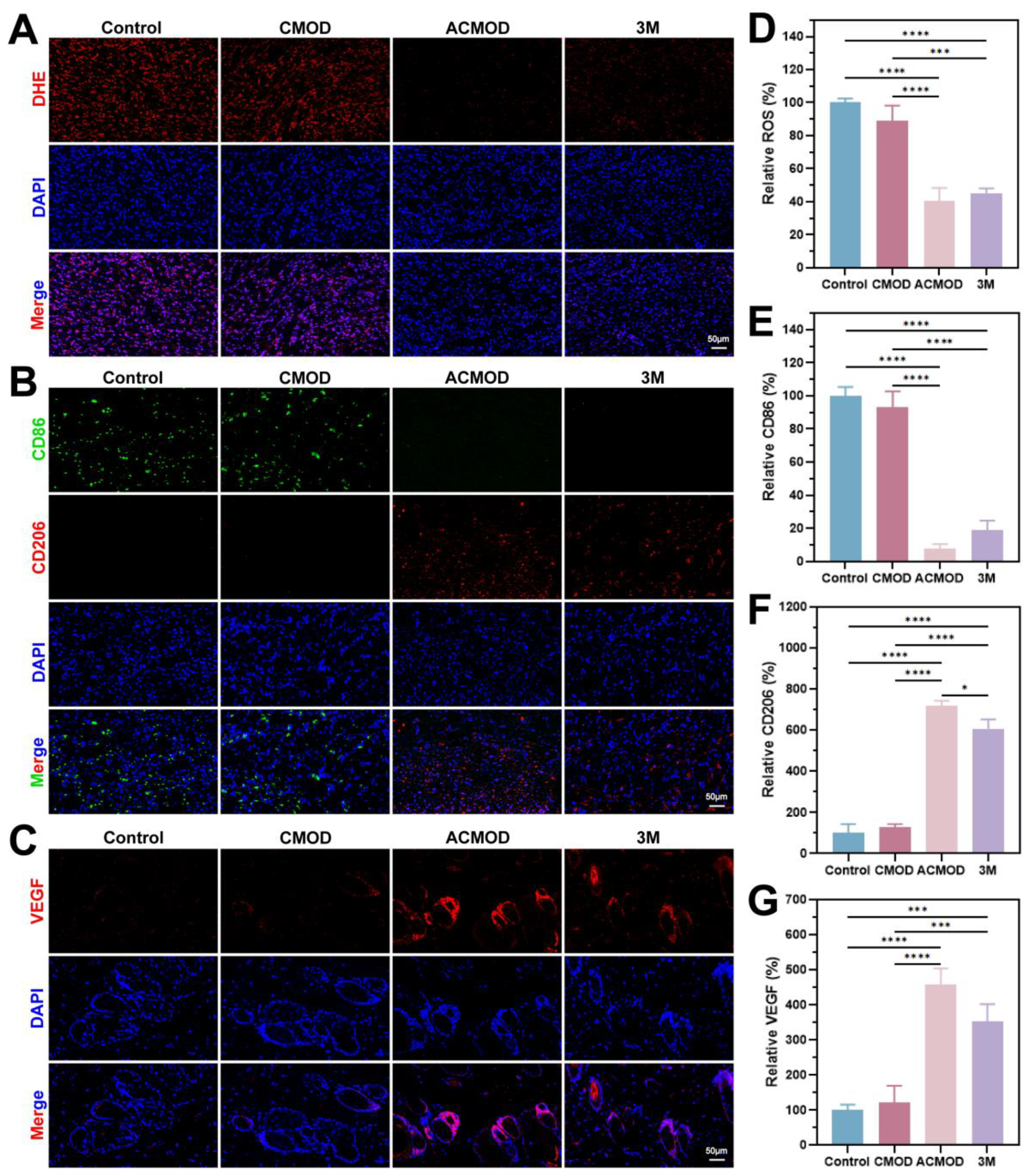
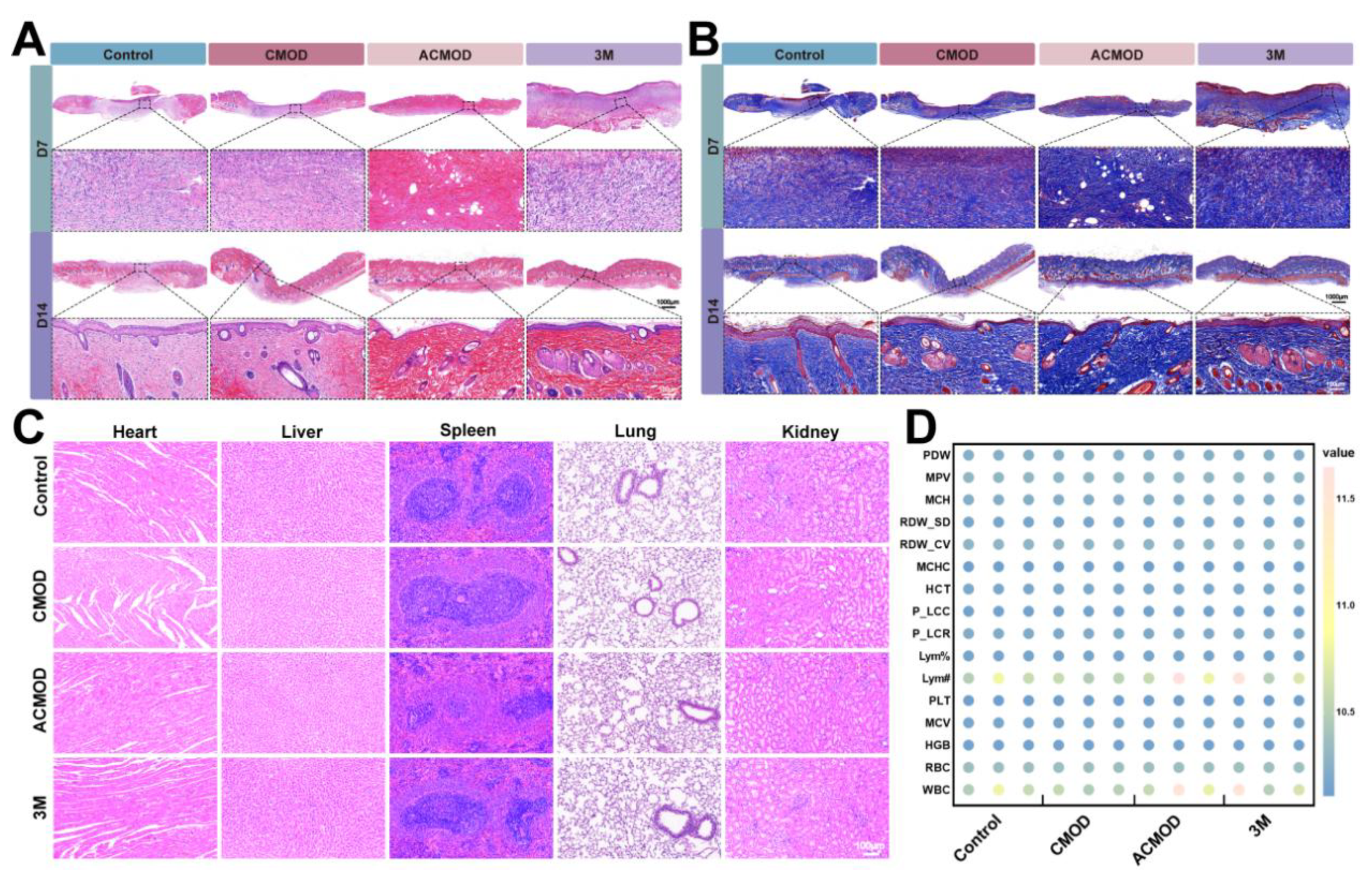
3.9. Immunofluorescence and Histological Analysis of Wound Tissues
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Zareie, P.; Weiss, E.S.; Kaplan, D.H.; Mackay, L.K. Cutaneous T cell immunity. Nat. Immunol. 2025, 26, 1014–1022. [Google Scholar] [CrossRef] [PubMed]
- Siu, W.S.; Ma, H.; Leung, P.C. Review on Current Advancements in Facilitation of Burn Wound Healing. Bioengineering 2025, 12, 428. [Google Scholar] [CrossRef]
- Wang, Z.; Qi, F.; Luo, H.; Xu, G.; Wang, D. Inflammatory Microenvironment of Skin Wounds. Front. Immunol. 2022, 13, 789274. [Google Scholar] [CrossRef]
- Noor, A.; Afzal, A.; Masood, R.; Khaliq, Z.; Ahmad, S.; Ahmad, F.; Qadir, M.-B.; Irfan, M. Dressings for burn wound: a review. J. Mater. Sci. 2022, 57, 6536–6572. [Google Scholar] [CrossRef]
- Craig, C.K.; Williams, J.W.; Carter, J.E.; Holmes, J.H. Bismuth/petroleum gauze plus high density polyethylene vs. bismuth/petroleum gauze: A comparison of donor site healing and patient comfort. Burns 2022, 48, 1917–1921. [Google Scholar] [CrossRef]
- Farahat, M.; Brosset, S.; Chen, Y.; Aijaz, A.; Rix, G.; Challagundla, B.; Elloso, M.; Hutter, M.F.; Rogers, I.M.; Jeschke, M.G. Human iPSCs-derived mesenchymal stem cells promote skin regeneration and burn wound healing. npj Regenerative Medicine 2025, 10, 40. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Pan, W.; Zhang, M.; Song, K.; Zhou, Z.; Zhao, Q.; Li, G.-Z.; Zhu, C. Chitosan-Based Dressing Materials for Burn Wound Healing. Polymers 2025, 17, 1647. [Google Scholar] [CrossRef]
- Ding, J.Y.; Xu, K.; Xu, H.T.; Ji, J.S.; Qian, Y.N.; Shen, J.L. Advances in Gas Therapeutics for Wound Healing: Mechanisms, Delivery Materials, and Prospects. Small Structures 2024, 5, 2300151. [Google Scholar] [CrossRef]
- Zhang, N.; Hu, P.; Wang, Y.; Tang, Q.; Zheng, Q.; Wang, Z.; He, Y. A Reactive Oxygen Species (ROS) Activated Hydrogen Sulfide (H2S) Donor with Self-Reporting Fluorescence. ACS Sensors 2020, 5, 319–326. [Google Scholar] [CrossRef]
- Lu, H.; Zeng, H.; Wei, W.; Chen, Y.; Zhou, Z.; Ning, X.; Hu, P. A fluorogenic ROS-triggered hydrogen sulfide donor for alleviating cerebral ischemia-reperfusion injury. Theranostics 2024, 14, 7589–7603. [Google Scholar] [CrossRef]
- Pandey, T.; Pandey, V. Hydrogen sulfide (H2S) metabolism: Unraveling cellular regulation, disease implications, and therapeutic prospects for precision medicine. Nitric Oxide 2024, 144, 20–28. [Google Scholar] [CrossRef]
- Lu, H.; Chen, Y.; Hu, P. Current Status and Future Prospects of Hydrogen Sulfide Donor-Based Delivery Systems. Advanced Therapeutics 2023, 6, 2200349. [Google Scholar] [CrossRef]
- Zeng, H.; Lu, H.; Yi, X.; Ning, X.; Lu, H.; Zhou, Z.; Liu, Z.; Zhou, X.; Hu, P. Nasal delivery of self-imaging ROS-responsive H₂S donors for enhanced neuroprotection in cerebral ischemia-reperfusion injury. Chemical Engineering Journal 2025, 519, 164934. [Google Scholar] [CrossRef]
- Stachowicz, A.; Czepiel, K.; Wiśniewska, A.; Stachyra, K.; Ulatowska-Białas, M.; Kuśnierz-Cabala, B.; Surmiak, M.; Majka, G.; Kuś, K.; Wood, M.E.; et al. Mitochondria-targeted hydrogen sulfide donor reduces fatty liver and obesity in mice fed a high fat diet by inhibiting de novo lipogenesis and inflammation via mTOR/SREBP-1 and NF-κB signaling pathways. Pharmacol. Res. 2024, 209, 107428. [Google Scholar] [CrossRef]
- Corsello, T.; Komaravelli, N.; Casola, A. Role of Hydrogen Sulfide in NRF2- and Sirtuin-Dependent Maintenance of Cellular Redox Balance. Antioxidants 2018, 7, 129. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.X.; Jing, M.R.; Cai, C.B.; Zhu, S.G.; Zhang, C.J.; Wang, Q.M.; Zhai, Y.K.; Ji, X.Y.; Wu, D.D. Role of hydrogen sulphide in physiological and pathological angiogenesis. Cell Prolif. 2022, 56, e13374. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Chen, X.; Liu, C.; He, Z.; Shen, Q.; Zhu, Y.; Wang, X.; Cao, S.; Yang, S. Endogenous hydrogen sulphide deficiency and exogenous hydrogen sulphide supplement regulate skin fibroblasts proliferation via necroptosis. Exp. Dermatol 2023, 33, e14972. [Google Scholar] [CrossRef] [PubMed]
- Cai, F.; Xu, H.; Cao, N.; Zhang, X.; Liu, J.; Lu, Y.; Chen, J.; Yang, Y.; Cheng, J.; Hua, Z.-C.; et al. ADT-OH, a hydrogen sulfide-releasing donor, induces apoptosis and inhibits the development of melanoma in vivo by upregulating FADD. Cell Death Dis. 2020, 11, 33. [Google Scholar] [CrossRef]
- Kasha, S.; Hanning, S.M.; Mugisho, O.O.; Thakur, S.S. Gas-based therapies in chronic wounds: A scoping review of preclinical and clinical data. Eur. J. Pharm. Biopharm. 2025, 217, 114894. [Google Scholar] [CrossRef]
- Shu, Q.; Gu, Y.; Xia, W.; Lu, X.; Pang, Y.; Teng, J.; Liu, B.; Li, Y. Injectable hydrogels for bioelectronics: A viable alternative to traditional hydrogels. Chemical Engineering Journal 2024, 495, 153391. [Google Scholar] [CrossRef]
- Xue, B.; Gu, J.; Li, L.; Yu, W.; Yin, S.; Qin, M.; Jiang, Q.; Wang, W.; Cao, Y. Hydrogel tapes for fault-tolerant strong wet adhesion. Nat. Commun 2021, 12, 7156. [Google Scholar] [CrossRef]
- Liang, Y.; Li, M.; Yang, Y.; Qiao, L.; Xu, H.; Guo, B. pH/Glucose Dual Responsive Metformin Release Hydrogel Dressings with Adhesion and Self-Healing via Dual-Dynamic Bonding for Athletic Diabetic Foot Wound Healing. ACS nano 2022, 16, 3194–3207. [Google Scholar] [CrossRef] [PubMed]
- Yuan, Y.; Shen, S.; Fan, D. A physicochemical double cross-linked multifunctional hydrogel for dynamic burn wound healing: shape adaptability, injectable self-healing property and enhanced adhesion. Biomaterials 2021, 276, 120838. [Google Scholar] [CrossRef] [PubMed]
- Mao, J.; Xiao, H.; Li, Y.; Wei, P.; Han, Y.; Tu, J.; Zhang, Z.; Xiao, Y.; Zhang, L. Self-healing, adhesive, hemostasis and anti-inflammation with a Schiff base-Crosslinked injectable hydrogel for burn wound healing. Appl. Mater. Today 2025, 46, 102906. [Google Scholar] [CrossRef]
- Hu, Y.; Yu, B.; Jia, Y.; Lei, M.; Li, Z.; Liu, H.; Huang, H.; Xu, F.; Li, J.; Wei, Z. Hyaluronate- and gelatin-based hydrogels encapsulating doxycycline as a wound dressing for burn injury therapy. Acta Biomater. 2023, 164, 151–158. [Google Scholar] [CrossRef]
- Wang, Z.; Liu, J.; Zheng, Y.; Zhang, B.; Hu, Y.; Wu, Y.; Li, Y.; Liu, L.; Zhu, H.; Liu, Q.; et al. Copper Ion-Inspired Dual Controllable Drug Release Hydrogels for Wound Management: Driven by Hydrogen Bonds. Small 2024, 20, e2401152. [Google Scholar] [CrossRef]
- Ning, X.; Lu, H.; Zeng, H.; Zhou, Z.; Hu, P. Multifunctional self-healing hydrogels for chronic wound repair: Design, mechanisms, and applications. J. Control. Release 2025, 388, 114282. [Google Scholar] [CrossRef]
- Zhou, Z.; Ning, X.; Wei, W.; Lu, H.; Wen, H.; Zeng, H.; Chen, Y.; Liu, J.; Xie, Y.; Hu, P. Dual-Network Hydrogel Loaded With ROS-activated Hydrogen Sulfide Donor to Accelerate Wound Healing and Inhibit Scar Production. Advanced Healthcare Materials 2025, 14, e2500264. [Google Scholar] [CrossRef] [PubMed]
- Shariatinia, Z. Carboxymethyl chitosan: Properties and biomedical applications. Int. J. Biol. Macromol. 2018, 120, 1406–1419. [Google Scholar] [CrossRef]
- Li, S.; Chen, N.; Li, X.; Li, Y.; Xie, Z.; Ma, Z.; Zhao, J.; Hou, X.; Yuan, X. Bioinspired Double-Dynamic-Bond Crosslinked Bioadhesive Enables Post-Wound Closure Care. Advanced Functional Materials 2020, 30, 2000130. [Google Scholar] [CrossRef]
- Zhou, Y.; Zhai, Z.; Yao, Y.; Stant, J.C.; Landrum, S.L.; Bortner, M.J.; Frazier, C.E.; Edgar, K.J. Oxidized hydroxypropyl cellulose/carboxymethyl chitosan hydrogels permit pH-responsive, targeted drug release. Carbohydr. Polym. 2023, 300, 120213. [Google Scholar] [CrossRef]
- Uberoi, A.; McCready-Vangi, A.; Grice, E.A. The wound microbiota: microbial mechanisms of impaired wound healing and infection. Nature Reviews Microbiology 2024, 22, 507–521. [Google Scholar] [CrossRef]
- Gong, L.; Chang, L.; Chen, S.; Wei, X.; Du, H.; Cheng, J.; Chen, X.; Yuan, Z.; Zhao, P.; Geng, M.; et al. Multifunctional injectable hydrogel with self-supplied H2S release and bacterial inhibition for the wound healing with enhanced macrophages polarization via interfering with PI3K/Akt pathway. Biomaterials 2025, 318, 123144. [Google Scholar] [CrossRef]
- Zhao, X.; Li, S.; Du, X.; Li, W.; Wang, Q.; He, D.; Yuan, J. Natural polymer-derived photocurable bioadhesive hydrogels for sutureless keratoplasty. Bioactive materials 2022, 8, 196–209. [Google Scholar] [CrossRef]
- Xu, L.; Zhou, Z.; Chen, Y.; Lu, H.; Hu, P. Resina Draconis Particles Encapsulated in a Hyaluronic-Acid-Based Hydrogel to Treat Complex Burn Wounds. Pharmaceutics 2022, 14, 2087. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Huang, Y.; Li, Z.; Chen, J.; Luo, J.; Bai, L.; Huang, H.; Cao, E.; Yin, Z.; Han, Y.; et al. Injectable Self-Expanding/Self-Propelling Hydrogel Adhesive with Procoagulant Activity and Rapid Gelation for Lethal Massive Hemorrhage Management. Adv. Mater. 2024, 36, e2308701. [Google Scholar] [CrossRef] [PubMed]
- Sahoo, M.; Sanklecha, R.; Mitra, D. Oxidized dextran-modified cotton gauze for application as a fouling-resistant wound dressing. Bull. Mater. Sci. 2024, 47, 269. [Google Scholar] [CrossRef]
- Sarkar, U.; Chattaraj, P.K. Reactivity Dynamics. The Journal of Physical Chemistry A 2021, 125, 2051–2060. [Google Scholar] [CrossRef]
- Shi, H.; Hu, C.; Li, A.; Lin, X.; Deng, M.; Jiang, B.; Xiao, B. Preparation of carboxymethylchitosan based rapid self-healing injectable hydrogels. Journal of Polymer Research 2023, 30, 342. [Google Scholar] [CrossRef]
- Yada, S.; Bazesefidpar, K.; Tammisola, O.; Amberg, G.; Bagheri, S. Rapid wetting of shear-thinning fluids. Physical Review Fluids 2023, 8, 043302. [Google Scholar] [CrossRef]
- Bao, H.; Zhang, C.; Pan, S.; Zhang, Z.; Yang, Y.; Li, S.; Wang, Y.; Wiedensohler, A. Quantitative description of self-, Maxwell–Stefan, and Fick diffusion coefficients in sucrose and citric acid solution based on molecular dynamics simulations. Physics of Fluids 2025, 37, 052013. [Google Scholar] [CrossRef]
- Lin, F.; Yang, Y.; Wei, S.; Huang, X.; Peng, Z.; Ke, X.; Zeng, Z.; Song, Y. Hydrogen Sulfide Protects Against High Glucose-Induced Human Umbilical Vein Endothelial Cell Injury Through Activating PI3K/Akt/eNOS Pathway. Drug Des. Devel. Ther. 2020, 14, 621–633. [Google Scholar] [CrossRef]
- Wang, L.; Miao, C.; Liang, F.; Shang, Y.; Sun, Y.; Zhang, J.; Shen, J.; Yin, M.; Yuan, J. Hydrogen sulfide releasing and carboxybetaine modified vascular graft with enhanced anticoagulant, anticalcification, and pro-endothelialization properties. Appl. Mater. Today 2023, 35, 101976. [Google Scholar] [CrossRef]
- Manna, S.; Gupta, S.M.; Bora, P.; Chakraborty, A.; Kumar, T.A.; Kamat, S.S.; Chakrapani, H. Tandem Biocatalysis to Generate Hydrogen Sulfide and Promote Endogenous Antioxidant Response. Angew. Chem. Int. Ed. 2025, 64, e202502917. [Google Scholar] [CrossRef]
- Wang, H.; Shi, X.; Qiu, M.; Lv, S.; Zheng, H.; Niu, B.; Liu, H. Hydrogen Sulfide Plays an Important Role by Influencing NLRP3 inflammasome. Int. J. Biol. Sci. 2020, 16, 2752–2760. [Google Scholar] [CrossRef]
- Chi, Z.; Chen, S.; Yang, D.; Cui, W.; Lu, Y.; Wang, Z.; Li, M.; Yu, W.; Zhang, J.; Jiang, Y.; et al. Gasdermin D-mediated metabolic crosstalk promotes tissue repair. Nature 2024, 634, 1168–1177. [Google Scholar] [CrossRef]
- Wang, C.; Liang, F.; Wang, L.; Sun, Y.; Xu, L.-C.; Zhang, J.; Pan, Y.; Shen, J.; Yin, M.; Yuan, J. Bilayer vascular grafts separately composited with nitric oxide-releasing keratin conjugates and hydrogen sulfide-releasing heparin conjugates. Int. J. Biol. Macromol. 2025, 307, 141887. [Google Scholar] [CrossRef]
- Alberts, A.; Bratu, A.G.; Niculescu, A.-G.; Grumezescu, A.M. Collagen-Based Wound Dressings: Innovations, Mechanisms, and Clinical Applications. Gels 2025, 11, 271. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.; Kim, M.-J.; Kumar, A.; Lee, H.-W.; Yang, Y.; Kim, Y. Vascular endothelial growth factor signaling in health and disease: from molecular mechanisms to therapeutic perspectives. Signal Transduction and Targeted Therapy 2025, 10, 170. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



