Submitted:
21 December 2023
Posted:
21 December 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Clinic and veterinarian selection:
Case selection
Pre-trial tutorial
Trial design
Data collection
Data analyses
3. Results
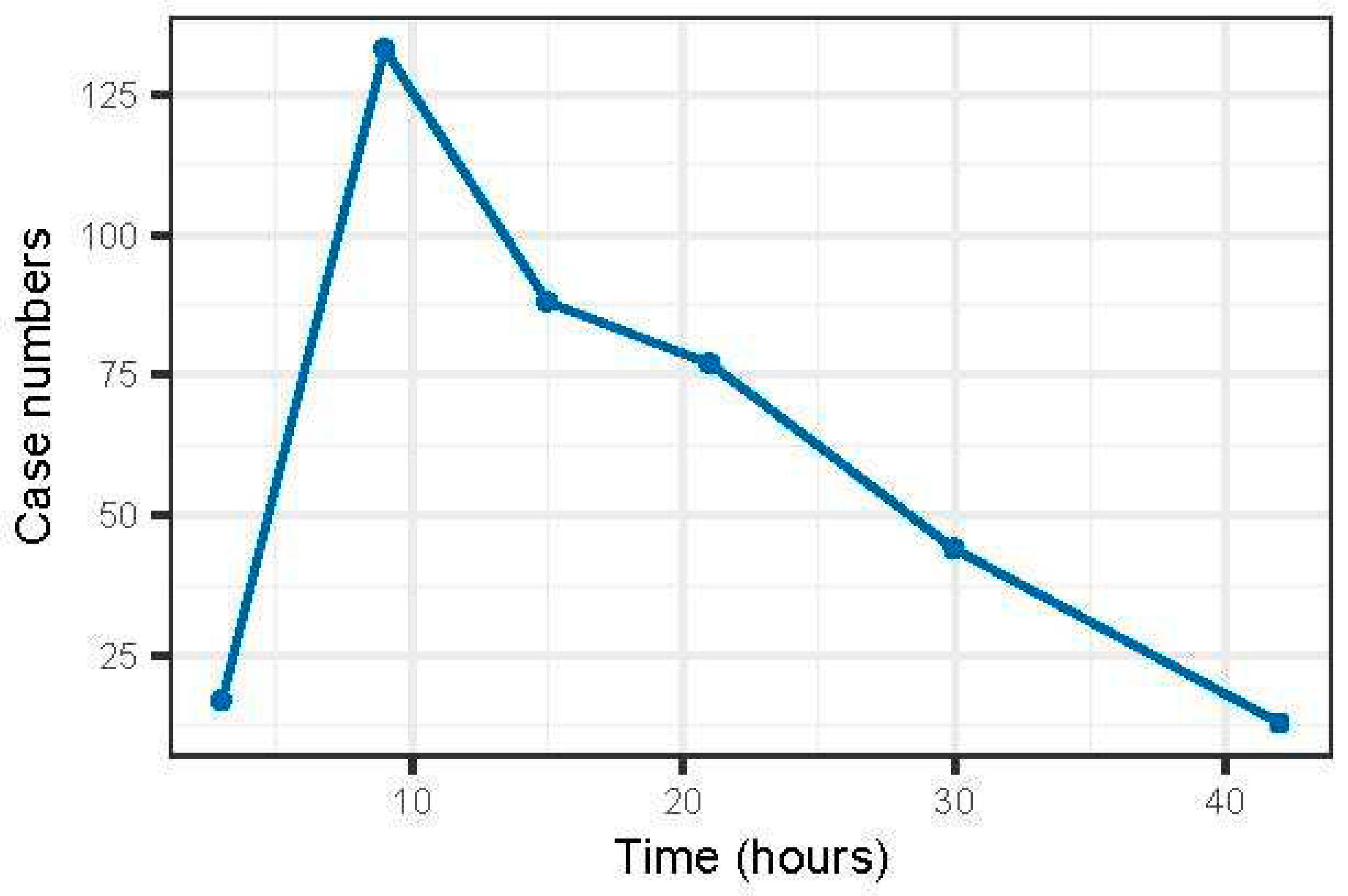
3.1. Descriptive data
3.2. Analyses
3.2.1. Animal and tick factors
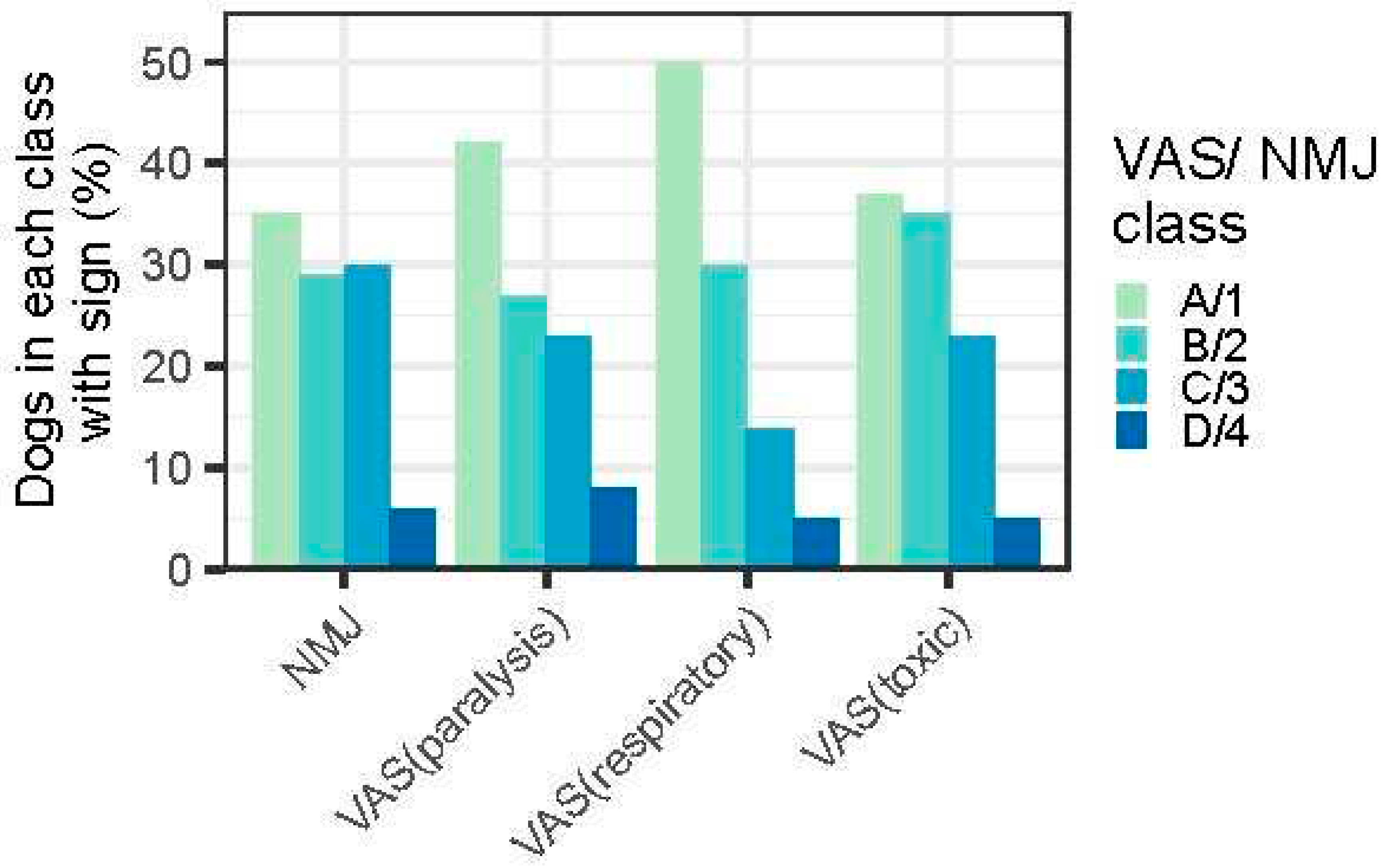
3.1.2. Predictors of outcome – NMJ and VAS
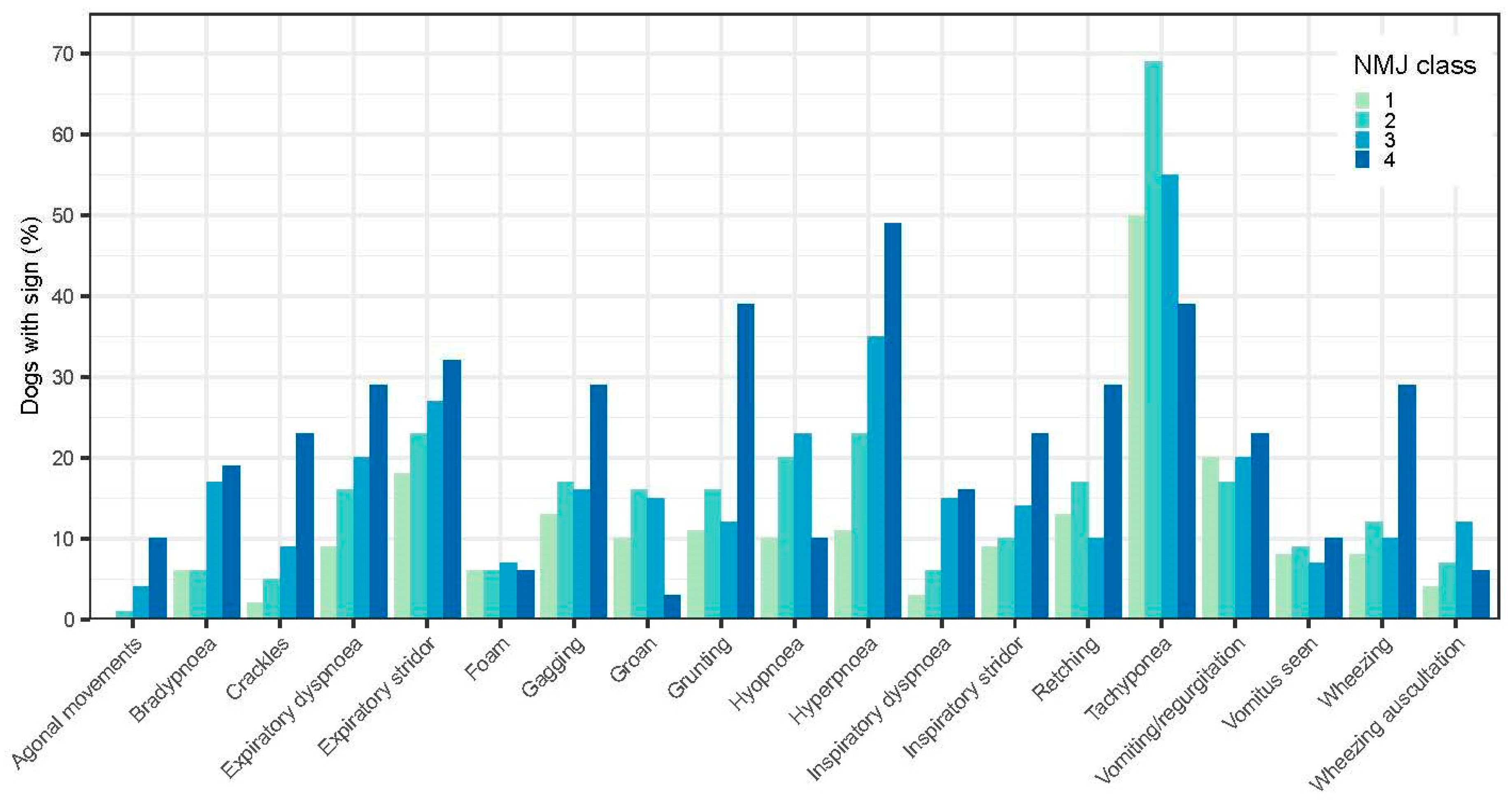
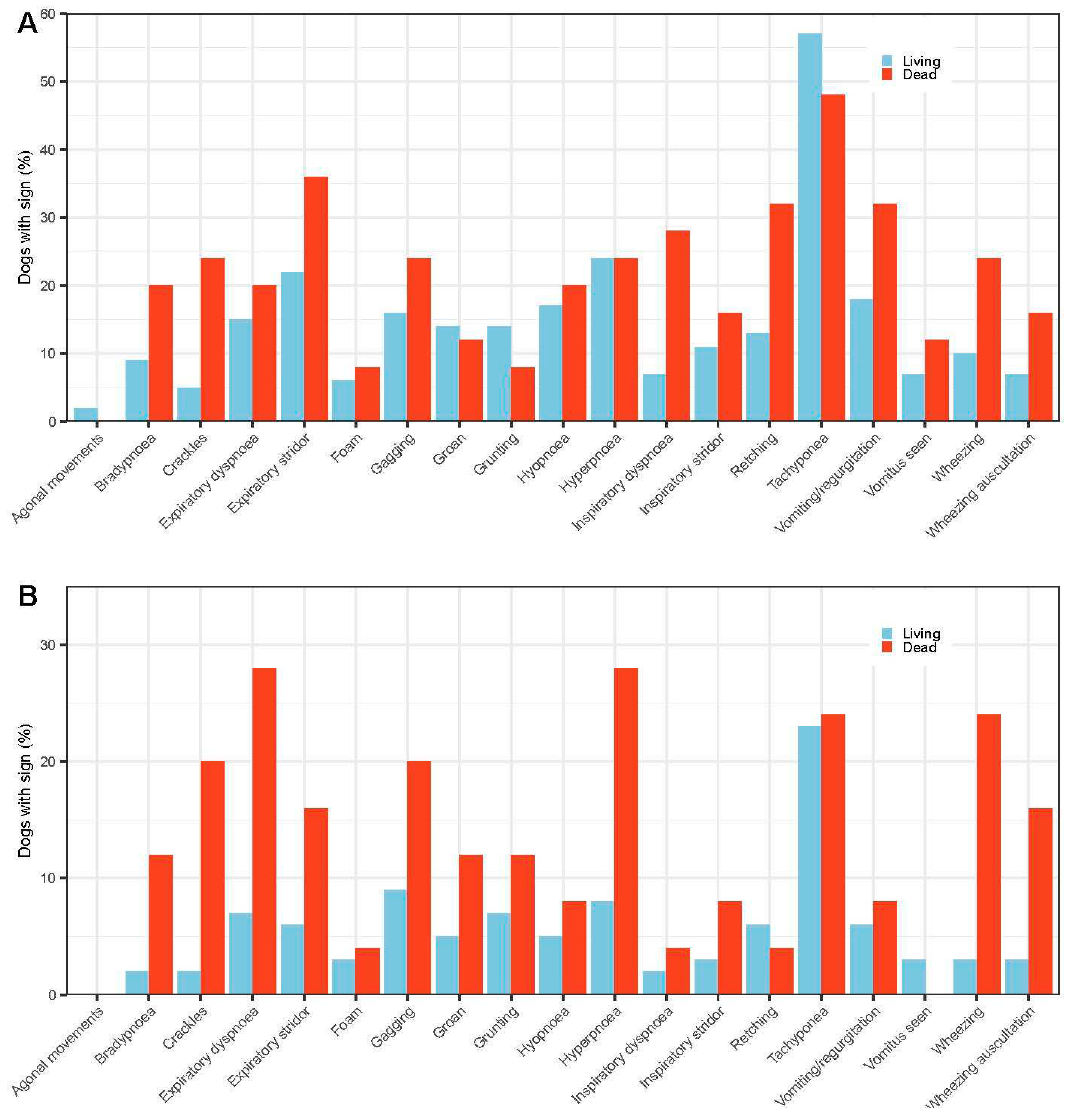
3.1.3. Predictors of outcome –specific clinical signs.
3.1.4. Predictors of outcome –facial expressions of distress
3.1.5. Geographic variation in clinical disease
3.1.6. Pharmaceutical product use and supportive treatments
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Statement
Acknowledgments
Conflicts of Interest
References
- Cooper, B.; Spence, I. Temperature-dependent inhibition of evoked acetylcholine release in tick paralysis. Nature 1976, 263, 693–695. [Google Scholar] [CrossRef] [PubMed]
- Ilkiw, J.E. A study of the effects in the dog of Ixodes holocyclus (PhD thesis), University of Sydney, NSW, 1979.
- Campbell, F.E.; Atwell, R.B. Heart failure in dogs with tick paralysis caused by the Australian paralysis tick, Ixodes holocyclus. Int J Appl Res Vet Med 2003, 1, 148–162. [Google Scholar]
- Fearnley, A. The importance of body temperature in the treatment of tick paralysis. Aust Vet Practit 2002, 32, 137–138. [Google Scholar]
- Schull, D.N.; O’Leary, C.A. The use of tick antitoxin serum and associated therapy for the treatment of dogs with Ixodes holocyclus toxicity. Aust Vet Practit 2007, 37, 90–97. [Google Scholar]
- Atwell, R.B. Tick Numbers in Different Dogs. Aust Vet Practit 2011, 41, 34–37. [Google Scholar]
- Atwell, R.B. Tick Studies – Some Observations. Aust Vet Practit 2007, 37, 121–122. [Google Scholar]
- Atwell, R.B. Tick Paralysis. The Merck Veterinary Manual 10th and 11th Edns. Merck & Coy Whitehouse Station NY USA, 2010.
- Atwell, R.B.; Campbell, F.E.; Evans, EA. Prospective survey of tick paralysis in dogs. Aust Vet J 2008, 79, 412–418. [Google Scholar] [CrossRef] [PubMed]
- Westwood, M.N.; Emery, D.L.; Dhand, N.K. Clinical presentation and treatment of tick paralysis in dogs and cats in Sydney (2001–2010). Aust Vet J 2013, 91, 491–498. [Google Scholar] [CrossRef] [PubMed]
- Atwell, R.B. Technical Bulletin – Tick Anti (Toxin) Serum – an Overview of Knowns and Unknowns. Merial, Sydney, 2010.
- Kunz, M.; Meixner, D.; Lautenbacher, S. Facial muscle movements encoding pain - a systematic review. Pain 2019, 160 (3), 535–549. [Google Scholar] [CrossRef]
- Prkachin, K.M. The consistency of facial expressions of pain: a comparison across modalities. Pain 1992, 51(3), 297–306. [Google Scholar] [CrossRef] [PubMed]
- McLennan, K.M.; Miller, A.L.; Dalla Costa, E.; Stucke, D.; Corke, M.J.; Broom, D.M.; Leach, M.C. Conceptual and methodological issues relating to pain assessment in mammals: The development and utilisation of pain facial expression scales. Appl Anim Beh Sci, 2019, 217, 1–15. [Google Scholar] [CrossRef]
- Sarolidou, G.; Axelsson, J.; Sundelin, T.; Lasselin, J.; Regenbogen, C.; Sorjonen, K.; Lundström, J.N.; Lekander, M.; Olsson, M.J. Emotional expressions of the sick face. Brain, Behavior, Immunity. 2019, 80, 286–291. [Google Scholar] [CrossRef] [PubMed]
- Langford, D.J.; Bailey, A.L.; Chanda, M.L.; Clarke, S.E.; Drummond, T.E.; Echols, S; Glick, S; Ingrao, J.; Klassen-Ross, T; LaCroix-Fralish, M.L; Matsumiya, L; Sorge, R.E.; Sotocinal, SG.; Tabaka, J.M.; Wong, D.; van den Maagdenberg, A.M.; Ferrari, M.D.; Craig, K.D.; Mogil, J.S. Coding of facial expressions of pain in the laboratory mouse. Nature Methods 2010, 7, 447–449. [Google Scholar] [CrossRef] [PubMed]
- McLennan, K.M.; Rebelo, Carlos J.B.; Corke, M.J.; Holmes, M.A. ; Leach, M.C.; Constantino-Casas, F. Development of a facial expression scale using footrot and mastitis as models of pain in sheep. Appl Anim Beh Sci 2016 176, 19-26. [CrossRef]
- Steiner, D.; Norman G. Health measurement scales: a practical guide to their development and use, 4th edn. Oxford 2008. [CrossRef]
- McCormack, H.; Horne, D.; Sheather, S. Clinical applications of visual analogue scales: a critical review. Psychol Med 1988, 18, 1007–1019. [Google Scholar] [CrossRef] [PubMed]
- Elera-Fitzcarrald, C.; Vega, K.; Gamboa-Cardenas, R.; Zuniga, K.; Zevallos, F.; Reategui-Sokolova, C.; Pastor-Asurza, C.; Perich-campos, R.; Bellido, Z.; Aranow, C.; Alarcon, G.; Calvo, A.; Ugarte-Gil, F. Reliability of visual analogue scale and numeric rating scale for the assessment of disease activity in systemic lupus erythematosus. J Clin. Rheum, 2020; 26(75), S170–S173. [Google Scholar] [CrossRef]
- Campbell, F.E.; Atwell, R.B. Reactions to tick antitoxin serum and the role of atropine in treatment of dogs and cats with tick paralysis caused by Ixodes holocyclus: a pilot survey. Aust Vet J. 2001, 79, 394–397. [Google Scholar] [CrossRef]
- Webster, R.A.; Mackie, J.T.; Haskins, S.T. Histopathological changes in the lungs from dogs with tick paralysis: 25 cases (2010–2012). Aust Vet J 2013, 91, 306–311. [Google Scholar] [CrossRef] [PubMed]
- Bloom, T.; Trevathan-Minnis, M.; Atlas, N.; MacDonald, D.A.; Friedman, H.L. Identifying facial expressions in dogs: A replication and extension study. Behavioural processes, 2021, 186, 104371–104371. [Google Scholar] [CrossRef] [PubMed]
- Song, S.; Shao, R.; Atwell, R.; Barker, S.; Vankan, D. Phylogenetic and phylogeographic relationships in Ixodes holocyclus and Ixodes cornuatus (Acari: Ixodidae) inferred from COX1and ITS2 gene sequences. Inter J Parasit 2011, 41, 871–880. [Google Scholar] [CrossRef] [PubMed]
- Cooper, B. Studies on the Pathogenesis of Tick Paralysis. (PhD Thesis), University of Sydney, NSW, 1976.
- Roidriguez-Valle, M; McAlister, S.; Moolhuijzen, P.; Booth, M.; Agnew, K.; Ellenberger, C.; Knowles, A.; Vanhoff, K.; Bellgard, M; Tabor, A. Immunomic investigation of Holocyclotoxins to produce the first protective anti-venom vaccine against the Australian paralysis tick, Ixodes holocyclus. Frontiers in Immunology 2021, 12, 744795. [Google Scholar] [CrossRef] [PubMed]
- Chand, K.; Lee, K.; Lavidis, N.; Rodriguez-Valle, M.; Ijaz, H.; Koehbach, J.; Clark, R.; Lew-Tabor, A.; Noakes, P. Tick holocyclotoxins trigger host paralysis by presynoptic inhibition. Scientific Reports 2016, 6(1), 29446. [Google Scholar] [CrossRef] [PubMed]
- Voight, D.; Gorb, S. Functional morphology of tarsal adhesive pads and attachment ability in ticks Ixodes ricinus (Arachnida, Acari. Ixodidae). J Exp Biol 2017, 220, 1984–1996. [Google Scholar] [CrossRef]
- Day, J.; Schull, D. Findings from Thoracic Radiographs of Dogs and Cats with Tick Toxicity. Aust Vet Practit. 2008, 38, 86–90. [Google Scholar]
| Factor | P-value |
|---|---|
| Tick number | 0.89 |
| Tick size | 0.97 |
| Whether ticks were plucked | 0.46 |
| Whether diagnosis was by presence of crater or tick | 0.63 |
| Whether ticks were alive or dead | 0.32 |
| Adult or non-adult stage of tick | 0.66 |
| Whether tick was located on presentation at clinics or removed at home prior to presentation | 0.18 |
| Whether tick detected by owner or by clinic | 0.46 |
| Cardiopulmonary disease | 0.37 |
| Other concurrent disease | 0.75 |
| Concurrent (non-tick) drug therapy | 0.77 |
| Scores | A1 OR (Mortality %) |
B2 OR (Mortality %) |
C3 OR (Mortality %) |
D4 OR (Mortality %) |
|---|---|---|---|---|
| VASTOXIC | 1 (3.1) | 0.6 (2) | 2.6 (7.8) | 19.9** (39.1)* |
| NMJ | 1 (3.2) | 0.5 (1.6) | 2.5 (7.6) | 14 (32) |
| VASPARAL | 1 (2.7) | 0.6 (1.7) | 2.7 (7) | 15.5 (30.3) |
| VASRESP | 1 (1.9) | 2.6 (4.7) | 6.6 (11.1) | 30.3** (36.4)* |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





