1. Introduction
The rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), causing coronavirus disease 2019 (COVID-19) pandemic, has resulted in distinct variants which are characterized by increased transmissibility, immune invasion strategies and replication advantages [
1]. The number of laboratory-confirmed COVID-19 cases has significantly increased especially following the emergence of BA.1, BA.2, BA.4 and BA.5 Omicron sublineages [
2].
SARS-CoV-2 confirmed cases in children younger than 18 years old have exceeded 16 million, according to American Academy of Pediatrics [
3]. Although viral transmission rates have been documented in various activities, including educational settings, children are most typically infected by close contact with an infected family member within the same household[
4].
Conventional approaches to acute disease surveillance fail to encompass the exact burden of COVID-19 due to factors such as asymptomatic, undetected, or unreported cases, especially in pediatric population, especially after Omicron emergence [
3]. Early studies in 2020 support that SARS-CoV-2 asymptomatic infection ratio in children ranges between 15-40% [
5]. A study from the United States in 2022 showed that SARS-CoV-2 asymptomatic infections in children during 2020 and 2021 reached 65% [
6].
Despite the predominance of different SARS-CoV-2 sublienages, SARS-CoV-2 antibody detection remains the most accurate test for SARS-CoV-2 infection confirmation. Serologic tests have limited utility for acute SARS-CoV-2 infection diagnosis [
7]. Antibody responses comprise the initial production of immunoglobulin M (IgM), which is subsequently followed by an increase in body circulation of IgA and IgG [
8]. The presence of IgG antibodies is typically detectable 16–20 days following infection in the majority of patients [
9]. A comprehensive analysis of 38 studies examining the accuracy of serologic testing in COVID-19 patients based on the duration of symptoms revealed that IgM antibodies were identified in 23% of cases within one week, 58% within two weeks, and 75% within three weeks. Similarly, IgG antibodies were detected in 30%, 66%, and 88% of cases, respectively [
10]. SARS-CoV-2 IgG nucleocapsid protein antibodies are produced only after natural infection and are not produced after SARS-CoV-2 vaccination, while SARS-CoV-2 IgG spike protein antibodies are produced both after natural infection and vaccination, since SARS-CoV-2 spike protein in the major antigenic target of currently available SARS-CoV-2 vaccines [
11]. Seroprevalence studies, based on SARS-CoV-2 natural infection antibodies, assist by determining a more accurate approach to COVID-19 proportion in pediatric population and offer valuable public health surveillance evidence [
12].
SARS-CoV-2 seropositivity was prospectively investigated in Athens metropolitan area pediatric population by our research group and highlighted the increase of SARS-CoV-2 seropositivity in children from Wuhan strain (1.7%) to Alpha (12.7%), Delta (29.7%) and pre-BA.5 Omicron predominance periods (48.5%) [
13,
14]. In these studies, the possible role of sex, age, origin, hospitalization status and different hospital departments on SARS-CoV-2 natural infection seropositivity and antibody levels was evaluated. The predominance period of BA.5. Omicron sublineage in Europe, including Greece, was approximately initiated on May 2022 [
15].
In current SARS-CoV-2 seroepidemiological study, we aim to investigate SARS-CoV-2 natural infection seropositivity and antibody levels during distinct BA.5 Omicron predominance subperiods and associate with epidemiological parameters.
2. Materials and Methods
2.1. Study Design and Participants
This is a prospective seroepidemiological study conducted at ‘'Aghia Sophia’’ Children's Hospital, the largest (750-bed) pediatric hospital in Greece and also a pediatric COVID-19 reference center for Athens metropolitan area. Subjects of the study were children 0-16 years old who were admitted to the hospital or presented to the emergency department for any reason other than confirmed SARS-CoV-2 infection.
To prospectively evaluate SARS-CoV-2 infection seropositivity and antibody levels, approximately 100 leftover sera per month were randomly collected from the Department of Biochemistry of ‘'Aghia Sophia’’ Children's Hospital. Serum samples were collected and stored at -70oC until laboratory analysis. Serum samples laboratory processes were performed anonymously using a unique individual identification code. When a child was readmitted to the hospital on multiple occasions during the study period and had positive antibody test results, only the initial positive result was included in the analysis. Children who were admitted to the Departments of Oncology, Bleeding Disorders, or β-Thalassemia were prospectively excluded from the study because of possible interference with antibody detection due to immunocompromised conditions or transfusions.
Demographic data of sex, age, origin (Greek, non-Greek), hospitalization status and hospital department [pediatric departments, emergency department, neonatal intensive care unit (NICU), pediatric intensive care unit (PICU), surgical departments (surgery, orthopedics, otorhinolaryngology, ophthalmology, urology, cardiothoracic surgery, neurosurgery and plastic surgery departments)] were also prospectively collected and included in analysis. Children of all ages were involved in the study and were classified as neonates and infants (0–1 year), toddlers (1–4 years), pre-school age children (4–6 years), school age children (6–12 years), and adolescents (12–16 years).
Due to high SARS-CoV-2 seropositivity rates detected in Athens in our last published seroepidemiology study by April 2022 [
14], we decided to perform follow-up SARS-CoV-2 seroprevalence studies every six months. Thus, the research timeframe was divided into three subperiods which corresponded to the predominance of SARS-CoV-2 BA.5 variant in Greece; period A: 01/05/2022-31/08/2022, period B: 01/09/2022-31/12/2022 and period C: July 2023.
The study protocol was in accordance with the 1964 Declaration of Helsinki and was approved by the scientific and bioethics committee of “Aghia Sophia” Children's Hospital (No. 25609).
2.2. SARS-CoV-2 Antibody Detection
Serum samples were analyzed for total SARS-CoV-2 nucleocapsid protein antibodies (Abs-N) for all the study period using Elecsys® Anti-SARS-CoV-2 (Roche Diagnostics, Basel, Switzerland) reagent [values of ≥1 cut-off index (COI) are positive]. During the last subperiod (July 2023) all children who were negative for Abs-N were also analyzed for spike protein antibodies (Abs-S) using Anti-SARS-CoV-2 S (Roche Diagnostics, Basel, Switzerland) reagent (values ≥ 0.8 U/mL are positive). The Cobas e 411 immunoassay analyzer and reagents were used according to manufacturer's instructions. Elecsys® Anti-SARS-CoV-2 is an electrochemiluminescence immunoassay (ECLIA) that use a double antigen sandwich enzyme-linked immunosorbent test technology. The ECLIA method is a highly efficient approach, with an estimated sensitivity of 99.5% (14 days after symptoms appear) and a specificity of 99.8%.
2.3. Statistical Analysis
Statistical analysis was performed using Statistical Package for the Social Sciences SPSS version 25.0 (IBM Corp., Released 2017. IBM SPSS Statistics for Windows, Version 25.0. IBM Corp). Absolute and relative frequencies (%) were used for the description of qualitative variables. Median and interquartile range (IQR) were applied for quantitative variables after the assumption of normality was evaluated with kurtosis and skewness and verified with Kolmogorov–Smirnov and Shapiro–Wilk tests. X2 tests were applied to assess distinctions among qualitative variables. Differences between qualitative and quantitative variables involved the application of two nonparametric tests: the Wilcoxon rank sum test (qualitative with 2 categories) and the Kruskal–Wallis test (qualitative with >2 categories). Correlations between quantitative variables were accessed via the Spearman r correlation coefficient. A multiple linear regression model was performed in order to estimate the SARS-CoV-2 seropositive children antibody titers (quantitative dependent variable) taking into account the simultaneous interaction of study period, age, sex, origin and hospitalization (independent variables). Graphs were created using GraphPad Prism 10. Statistical significance was set at a P-value of <0.05 level.
4. Discussion
In the present study, we investigated SARS-CoV-2 seropositivity and antibody levels during BA.5 predominance period in Athens pediatric population taking into consideration epidemiological parameters. This is a follow-up study from previous investigations starting from the beginning of the pandemic (3/2020) showing a gradual increase in seropositivity rates in our area from 4% to 52.6% [
13,
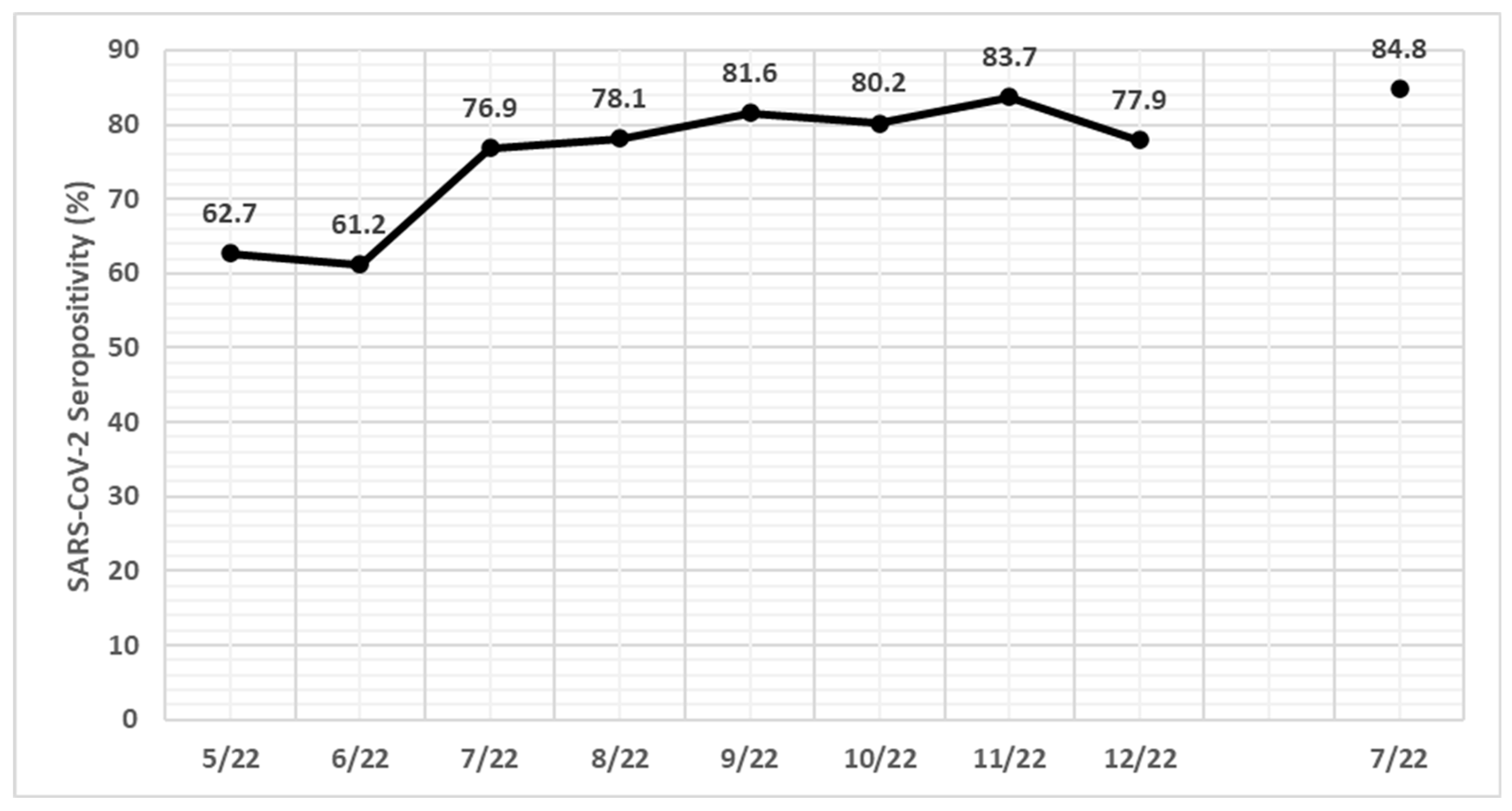
14]. A further increase in SARS-CoV-2 Abs-N seropositivity during BA.5 predominance period from 62.7% in May 2022 to 84.8% in July 2023 was detected. SARS-CoV-2 seropositivity increased for all age groups, for both sexes, regardless of origin or hospitalization status, and in all different hospital departments, including emergency departments.
The prospective acquisition of routine leftover residual serum samples from the Biochemistry department presents a viable approach for assessing SARS-CoV-2 serosurveillance in children and provides the advantage of avoiding additional blood sampling for paediatric patients. All previous studies were based on the testing of routine leftover residual serum samples avoiding additional blood sampling for pediatric patients and has successfully been implemented in other seroprevalence studies as well [
17,
18,
19].
SARS-CoV-2 seropositivity in our area does not substantially differ from reported seroepidemiological data from the USA, Latvia, Thailand, Guinea and Cameroon, indicating increased SARS-CoV-2 seropositivity during the BA.5 Omicron period [
18,
20,
21,
22]. No differences in SARS-CoV-2 seropositivity rates between sexes was detected which is also the finding of Greek National Public Health Organization COVID-19 Surveillance System and other similar studies [
15], [
17,
18]. According to our previously published studies, SARS-CoV-2 seropositivity rates between sexes did not significantly differ either during Wuhan (females: 1.4% vs males: 1.4%), or Alpha (females: 14.6% vs males: 19.7%), or Delta (females: 32.8% vs males: 27.3%) or pre-BA.5 Omicron (females: 47.7% vs males: 49.2%) predominance periods, respectively [
13,
14].
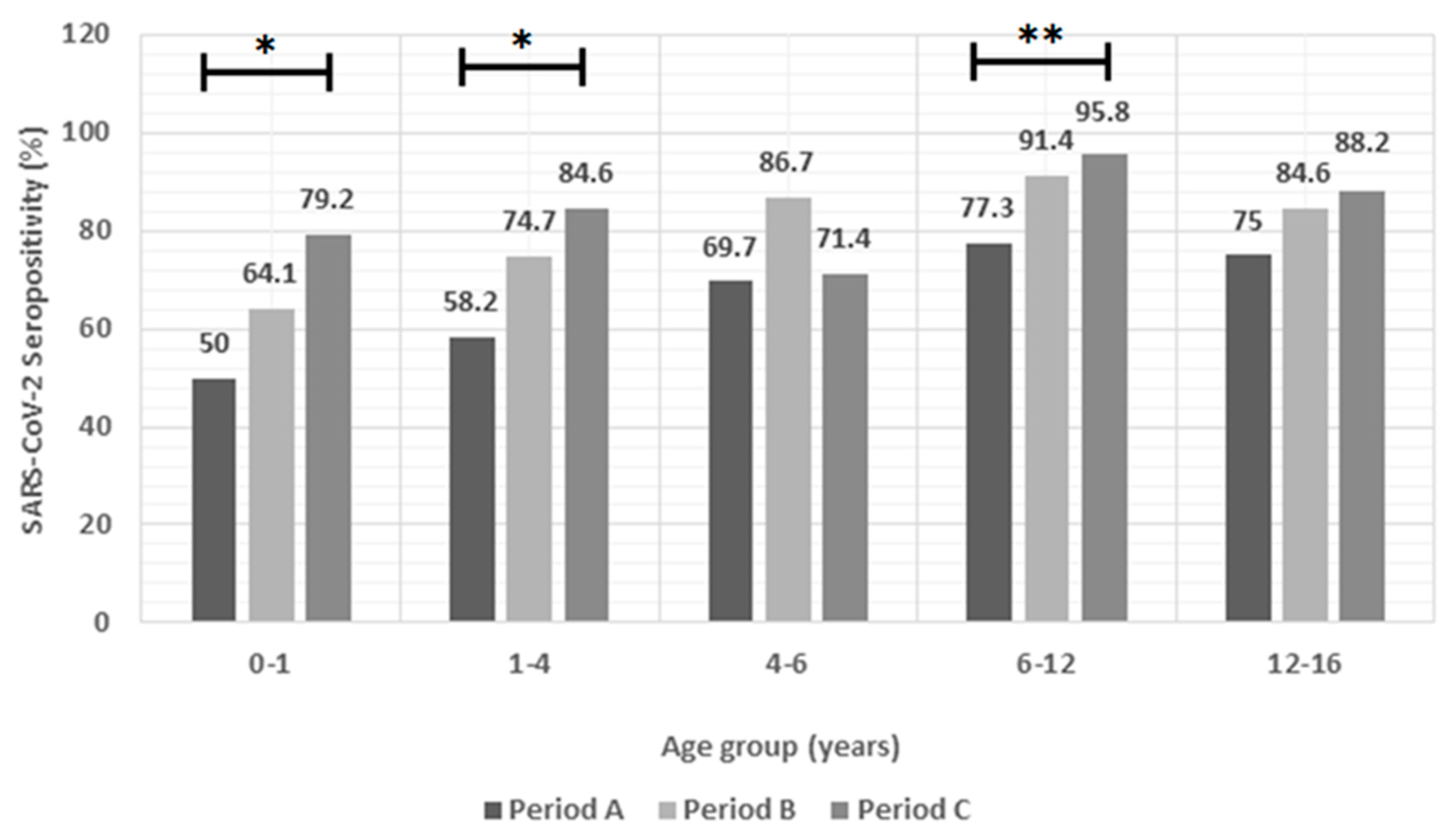
In this study, SARS-CoV-2 infection seropositivity increased for all age groups and was higher especially for children 6-12 years and adolescents (12-16 years). Similar findings from CDC report that children 5-11 years old, from May to October 2022 in USA, had the highest SARS-CoV-2 natural infection seropositivity rates (93.5%) follower by 12-17 years (93%) [
22]. According to our previously published studies, SARS-CoV-2 natural infection seropositivity rates in children 6-12 years gradually increased from 0% in Wuhan to 14.4% in Alpha, 27.8% in Delta and 56.5% in pre-BA.5 Omicron predominance periods [
13,
14]. Similarly, SARS-CoV-2 seropositivity rates in children 12-16 years increased from 0% in Wuhan to 16.9% in Alpha, 32.5% in Delta and 51.8% in pre-BA.5 Omicron predominance periods, respectively [
13,
14].
A SARS-CoV-2 seropositivity study in Latvia from May 2022 to July 2022 in 173 children showed that children 12-18 years had the highest seropositivity rates (94.3%) when compared to 5-11 years (90.9%) and <5 years (77.8%) [
20]. These differences could possibly be attributed to different number of participants and age group stratification. These findings may be attributed to the increased exposure of school-age children in Omicron period and enhanced transmissibility of BA.5 subvariant.
According to a recent meta-analysis, SARS-CoV-2 seropositivity is higher in children of Asian and African regions [
23]. These countries are also associated with increased migration rates to Greece over the last years. In the present study, children of non-Greek origin had similar seropositivity in contrast with the findings from our previously published data in 2021 and 2022 [
13,
14]. In our previously published studies, SARS-CoV-2 seropositivity rates significantly differed between Greek and non-Greek children during Wuhan (Greek: 1% vs non-Greek: 2.4%) and Alpha (Greek: 14.3% vs non-Greek: 25.6%) but not during Delta (Greek: 29.3% vs non-Greek: 31.5%) or pre-BA.5 Omicron (Greek: 48% vs non-Greek: 49.7%) predominance periods, respectively [
13], [
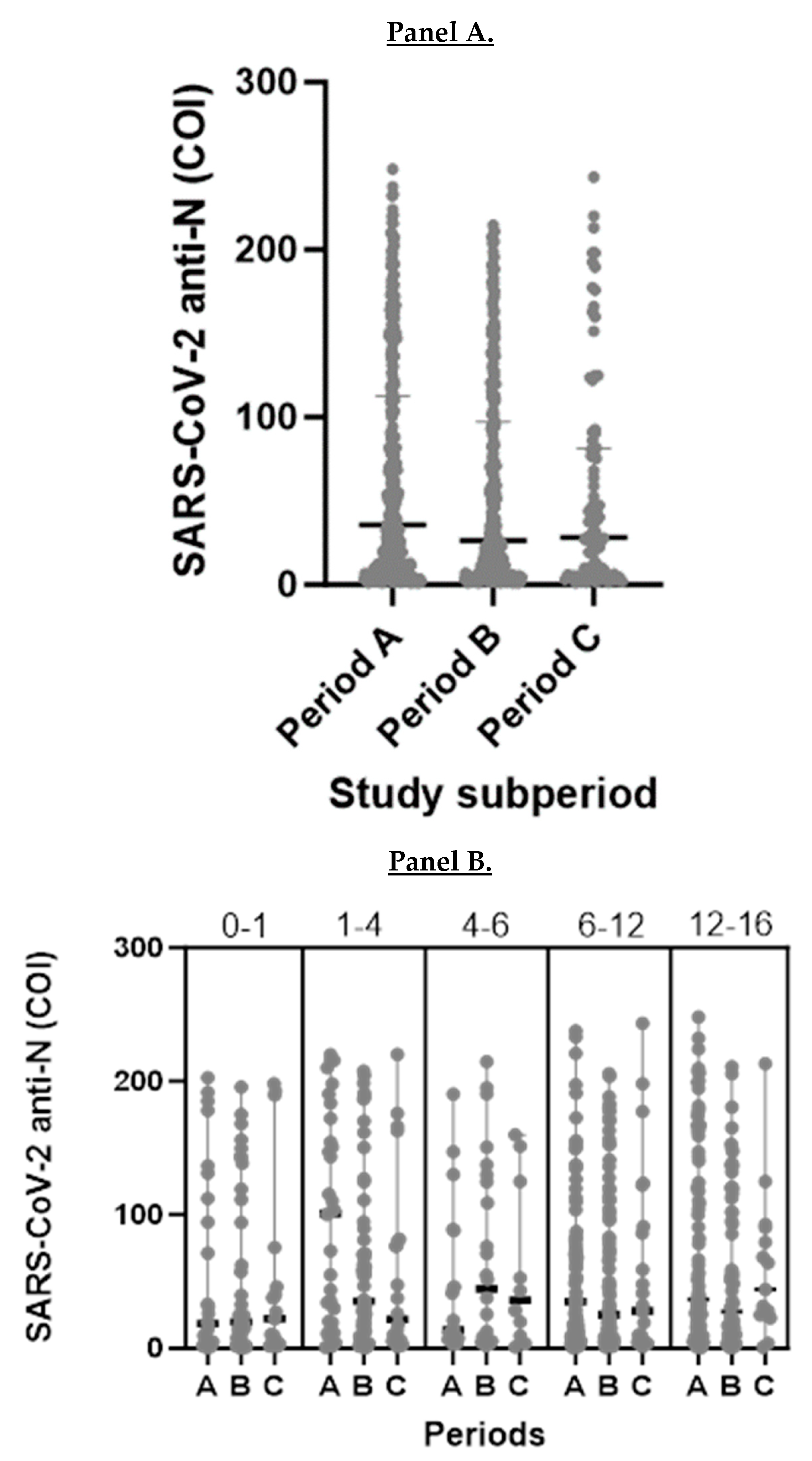
14]. However, in current study, children of non-Greek origin had higher antibody titers compared to Greek. This finding could possibly indicate increased exposure that leads to repeated infections among non-Greek underprivileged communities within Athens metropolitan area.
Due to high SARS-CoV-2 seropositivity rates for natural infection (Abs-N) in our area, we decided to perform follow-up SARS-CoV-2 seroprevalence studies every six months with additional Abs-S testing. From the additional testing, it was shown that even with negative Abs-N a significant percentage of population could have positive Abs-S representing either immunization or SARS-CoV-2 exposure. After detecting both antibodies, it was found that children 6-16 years had 100% SARS-CoV-2 seropositivity. According to CDC, these two pediatric age groups are associated with the highest seroprevalence rates (97.1% for school-age children and 98.9% for adolescents, respectively) and agree with the findings of our study [
22]. In Greece, where approximately half of total country population has laboratory-confirmed COVID-19, SARS-CoV-2 vaccination rates with a complete primary series reach 75% in adults and children[
24]. Waning Humoral immunity several months following SARS-CoV-2 infection [
25] supports that SARS-CoV-2 vaccination is of vital importance to offer a surrogate of protection. Our data suggest that, in future seroepidemiological studies, both antibodies should be tested in Abs-N seronegative population.
In Winter 2022 BA.5 predominance period, non-hospitalized children were incommensurately affected by COVID-19 compared to hospitalized children regardless of different hospital departments. In contrast, hospitalized children in Greece were found to have higher seropositivity rates during Alpha and Delta periods [
13,
14]. Those differences could be explained as more children possibly visited the emergency department during Omicron for mild common cold symptoms due to SARS-CoV-2 reinfection but were not detected as SARS-CoV-2 positive at admission by molecular or rapid antigen testing. This hypothesis could also explain the increased antibody titers of non-hospitalized compared to hospitalized children also reported in our study. According to CDC, there is an increasing trend of emergency department visits due to COVID-19 diagnosis during 2023 for both children and adults [
26]. Therefore, SARS-CoV-2 seroprevalence studies in different hospital departments, including emergency departments, could provide valuable epidemiological data or possibly guide hospital measures.
Limitations of present study include that it represents data from a specific area of Greece and not in a national level. In addition, Abs-N, representing natural infection, was analyzed for the total population and Abs-S, which could be also vaccine-induced, was additionally analyzed only for the last period of the study. The suggested multiple linear regression model for SARS-CoV-2 antibody titers was successful for antibody values measured only by a certain detection laboratory assay and should be interpreted cautiously if applied to other distinct assays. Therefore, the ultimate trajectory of bias arising from these factors remains uncertain. However, this is the third part of our department’s prospective longitudinal seroepidemiology and antibody levels study from the beginning of the pandemic involving the pediatric population of Athens metropolitan area and it is the largest in terms of duration (2020-2022) and total study population (approximately 5000 children 0-16 years old in total) in Greece.
Author Contributions
Conceptualization, A.M. and V.S.; methodology, A.M., V.S. and F.F.; validation, F.F., E.-B.T. and A.M.; formal analysis, F.F.; investigation, F.F. and E.-B.T.; data curation, F.F., M.-M.D. and Al.M.; writing—original draft preparation, F.F.; writing—review and editing, A.M. and V.S,; supervision, A.M..; project administration, A.M. and F.F. All authors have read and agreed to the published version of the manuscript.