Submitted:
06 February 2024
Posted:
08 February 2024
You are already at the latest version
Abstract
Keywords:
Introduction
- Phase I: Clinical phase
- Phase II: Outpatient Cardiac Rehab
- Phase III: Post-Cardiac Rehab
Method
Study Design
Data Sources
Study Selection
Data Synthesis and Analysis
Ethical Consideration
Results
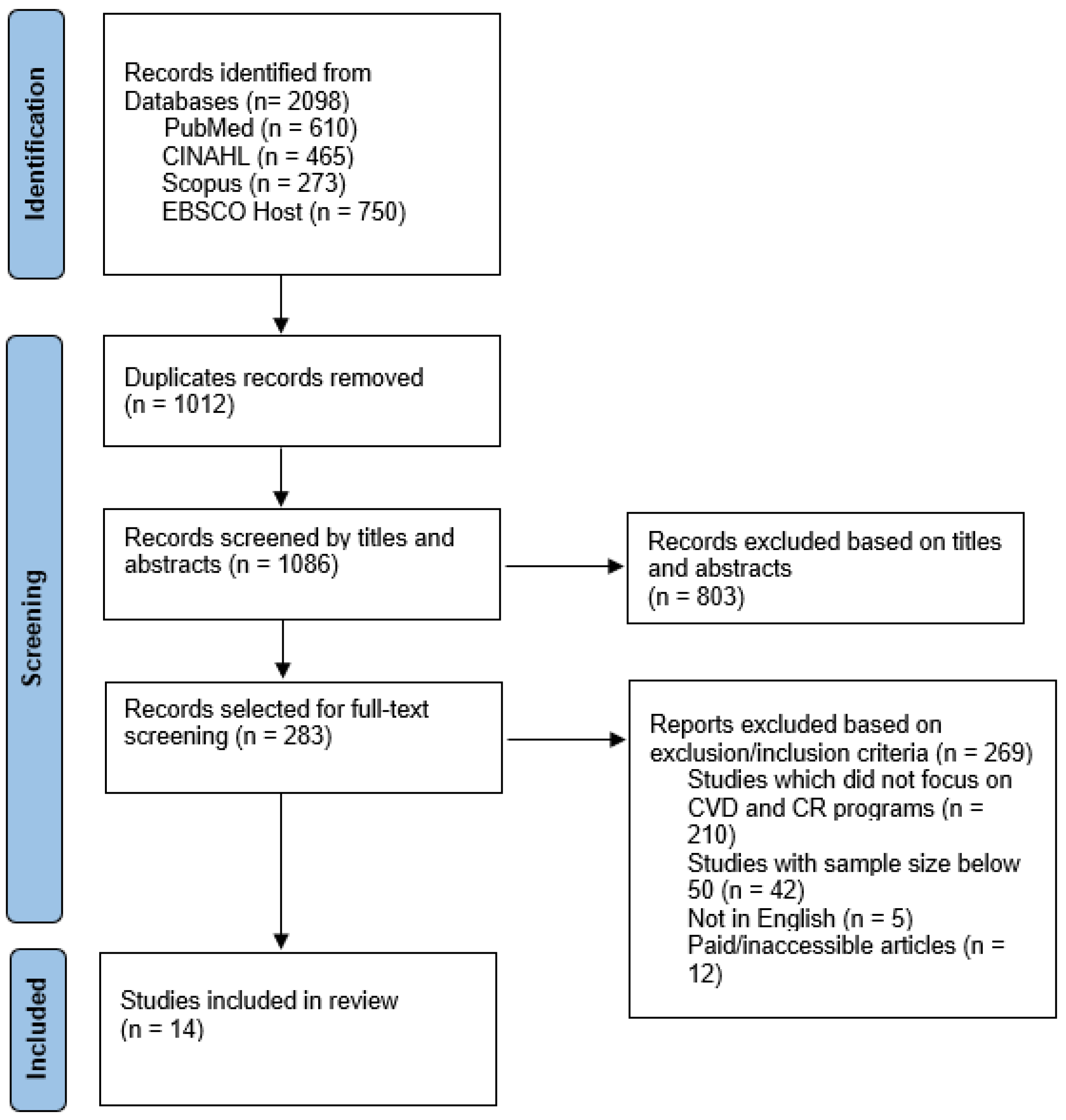
Identification and Selection of Literature
Healthcare System Related Factors
Availability of Cardiac Rehabilitation Programs
Referral Strategies
Inter-Provider Communication
Socio-Spatial Factors
Accessibility to Cardiac Rehabilitation Facilities
Employment Status/Income
Level of Education
Affordability and Access to Care
Individual Characteristics
Comorbidities
Generic Factors
Discussion
Limitations
Recommendation
Conclusion
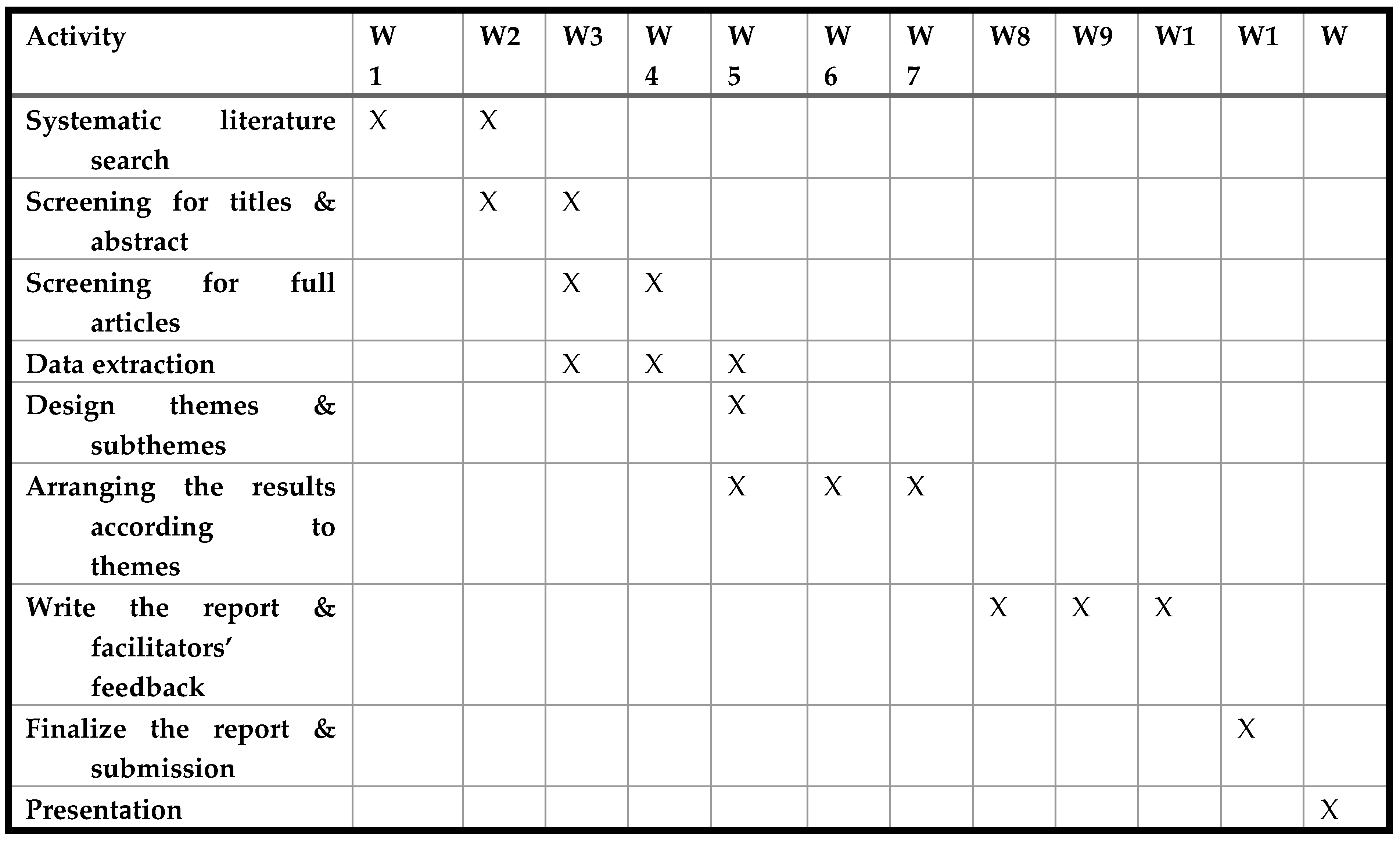
Gantt Chart
Contributions
Acknowledgments
Competing Interests (Disclosures/Sources of Funding)
References
- Anderson, L., & Taylor, R. S. (2014). Cardiac rehabilitation for people with heart disease: an overview of Cochrane systematic reviews. The Cochrane database of systematic reviews, 2014(12), CD011273-CD011273. [CrossRef]
- Bachmann, J. M., Huang, S., Gupta, D. K., Lipworth, L., Mumma, M. T., Blot, W. J., . . . Freiberg, M. S. (2017). Association of Neighborhood Socioeconomic Context With Participation in Cardiac Rehabilitation. Journal of the American Heart Association, 6(10), e006260. [CrossRef]
- Beckie, T. M., & Beckstead, J. W. (2010). Predicting cardiac rehabilitation attendance in a gender-tailored randomized clinical trial. Journal of Cardiopulmonary Rehabilitation and Prevention, 30(3), 147-156. [CrossRef]
- Bethell, H. J. N., Lewin, R. J. P., & Dalal, H. M. (2008). Cardiac rehabilitation: it works so why isn't it done? The British journal of general practice : the journal of the Royal College of General Practitioners, 58(555), 677-679. [CrossRef]
- Bloom, D. E., Chisholm, D., Jané-Llopis, E., Prettner, K., Stein, A., & Feigl, A. (2011). From Burden to “Best Buys”: Reducing the Economic Impact of Non-Communicable Diseases. World Health Org., Geneva, Switzerland.
- Borg, S., Öberg, B., Leosdottir, M., Lindolm, D., Nilsson, L., & Bäck, M. (2019). Factors associated with non-attendance at exercise-based cardiac rehabilitation. BMC sports science, medicine & rehabilitation, 11, 13-13. [CrossRef]
- Chamosa, S., Alarcón, J. A., Dorronsoro, M., Madruga, F. J., Barrera, J., Arrazola, X., . . . San Vicente, J. M. (2015). Predictors of Enrollment in Cardiac Rehabilitation Programs in Spain. Journal of Cardiopulmonary Rehabilitation and Prevention.
- , 35(4), 255-262. [CrossRef]
- Cieza, A., Causey, K., Kamenov, K., Hanson, S. W., Chatterji, S., & Vos, T. (2020). Global estimates of the need for rehabilitation based on the Global Burden of Disease study 2019: a systematic analysis for the Global Burden of Disease Study 2019. The Lancet, 396(10267), 2006-2017. [CrossRef]
- Darin-Mattsson, A., Fors, S., & Kåreholt, I. (2017). Different indicators of socioeconomic status and their relative importance as determinants of health in old age. International Journal for Equity in Health, 16(1), 173. [CrossRef]
- Davidson, P., Digiacomo, M., Zecchin, R., Clarke, M., Paul, G., Lamb, K., . . . Daly, J. (2008). A cardiac rehabilitation program to improve psychosocial outcomes of women with heart disease. J Womens Health (Larchmt), 17(1), 123-134. [CrossRef]
- Demmler, J. C., Hill, R. A., Rahman, M. A., Bandyopadhyay, A., Healy, M. A., Paranjothy, S., . . . Brophy, S. T. (2017). Educational Attainment at Age 10-11 Years Predicts Health Risk Behaviors and Injury Risk During Adolescence. The Journal of adolescent health : official publication of the Society for Adolescent Medicine, 61(2), 212-218. [CrossRef]
- Gaalema, D. E., Cutler, A. Y., Higgins, S. T., & Ades, P. A. (2015). Smoking and cardiac rehabilitation participation: Associations with referral, attendance and adherence. Preventive medicine, 80, 67-74. [CrossRef]
- Ge, C., Ma, J., Xu, Y., Shi, Y.-J., Zhao, C.-H., Gao, L., . . . Chen, Y.-D. (2019). Predictors of adherence to home-based cardiac rehabilitation program among coronary artery disease outpatients in China. Journal of geriatric cardiology : JGC, 16(10), 749-755. [CrossRef]
- Gheorghe, A., Griffiths, U., Murphy, A., Legido-Quigley, H., Lamptey, P., & Perel, P. (2018). The economic burden of cardiovascular disease and hypertension in low- and middle-income countries: a systematic review. BMC Public Health, 18(1), 975. [CrossRef]
- Grace, S. L., Russell, K. L., Reid, R. D., Oh, P., Anand, S., Rush, J., . . . Stewart, D. E. (2011). Effect of cardiac rehabilitation referral strategies on utilization rates: a prospective, controlled study. Arch Intern Med, 171(3), 235-241. [CrossRef]
- Grace, S. L., Russell, K. L., Reid, R. D., Oh, P., Anand, S., Rush, J., . . . Cardiac Rehabilitation Care Continuity Through Automatic Referral Evaluation, I. (2011). Effect of Cardiac Rehabilitation Referral Strategies on Utilization Rates: A Prospective, Controlled Study. Archives of Internal Medicine, 171(3), 235-241. [CrossRef]
- Gravely, S., Leung, Y., Nariani, R., Tamim, H., Oh, P., Chan, V., & Grace, S. (2009). Effects of cardiac rehabilitation referral strategies on referral and enrollment r. Nature reviews. Cardiology, 7, 87-96. [CrossRef]
- Fraser, M. J., Leslie, S. J., Gorely, T., Foster, E., & Walters, R. (2022). Barriers and facilitators to participating in cardiac rehabilitation and physical activity: A cross-sectional survey. World journal of cardiology, 14(2), 83–95. [CrossRef]
- Krishnamurthi, N., Schopfer, D. W., Shen, H., & Whooley, M. A. (2019). Association of Mental Health Conditions With Participation in Cardiac Rehabilitation. J Am Heart Assoc, 8(11), e011639. [CrossRef]
- Lavie, C. J., & Milani, R. V. (2001). Benefits of cardiac rehabilitation and exercise training programs in elderly coronary patients. Am J Geriatr Cardiol, 10(6), 323-327. [CrossRef]
- Liu, C., Wang, D., Liu, C., Jiang, J., Wang, X., Chen, H., . . . Zhang, X. (2020). What is the meaning of health literacy? A systematic review and qualitative synthesis. Family Medicine and Community Health, 8(2), e000351. [CrossRef]
- Moradi, B., Maleki, M., Esmaeilzadeh, M., & Abkenar, H. B. (2011). Physician-related factors affecting cardiac rehabilitation referral. The journal of Tehran Heart Center, 6(4), 187-192. Retrieved from https://pubmed.ncbi.nlm.nih.gov/23074367.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3467958/.
- Parashar, S., Spertus, J. A., Tang, F., Bishop, K. L., Vaccarino, V., Jackson, C. F., . . . Sperling, L. (2012). Predictors of Early and Late Enrollment in Cardiac Rehabilitation, Among Those Referred, After Acute Myocardial Infarction. Circulation, 126(13), 1587-1595. [CrossRef]
- Pesah, E., Turk-Adawi, K., Supervia, M., Lopez-Jimenez, F., Britto, R., Ding, R., . . . Grace, S. L. (2019). Cardiac rehabilitation delivery in low/middle-income countries. Heart (British Cardiac Society), 105(23), 1806-1812. [CrossRef]
- Pesah, E., Turk-Adawi, K., Supervia Pola, M., Lopez-Jimenez, F., Britto, R., Ding, R., . . . Grace, S. (2019). Cardiac rehabilitation delivery in low/middle-income countries. Heart, 105, heartjnl-2018. [CrossRef]
- Prabhu, N. V., Maiya, A. G., & Prabhu, N. S. (2020). Impact of Cardiac Rehabilitation on Functional Capacity and Physical Activity after Coronary Revascularization: A Scientific Review. Cardiology research and practice, 2020, 1236968-1236968. [CrossRef]
- Rodrigo, S. F., Van Exel, H. J., Van Keulen, N., Van Winden, L., Beeres, S. L. M. A., & Schalij, M. J. (2021). Referral and participation in cardiac rehabilitation of patients following acute coronary syndrome; lessons learned. IJC Heart & Vasculature, 36, 100858. [CrossRef]
- Roth, G. A., Mensah, G. A., Johnson, C. O., Addolorato, G., Ammirati, E., Baddour, L. M., . . . Fuster, V. (2020). Global Burden of Cardiovascular Diseases and Risk Factors, 1990–2019: Update From the GBD 2019 Study. Journal of the American College of Cardiology, 76(25), 2982-3021. [CrossRef]
- Schopfer, D. W., Priano, S., Allsup, K., Helfrich, C. D., Ho, P. M., Rumsfeld, J. S., . . . Whooley, M. A. (2016). Factors Associated With Utilization of Cardiac Rehabilitation Among Patients With Ischemic Heart Disease in the Veterans Health Administration: A QUALITATIVE STUDY. J Cardiopulm Rehabil Prev, 36(3), 167-173. [CrossRef]
- Shields, G. E., Wells, A., Doherty, P., Heagerty, A., Buck, D., & Davies, L. M. (2018). Cost-effectiveness of cardiac rehabilitation: a systematic review. Heart (British Cardiac Society), 104(17), 1403-1410. [CrossRef]
- Soroush, A., Heydarpour, B., Komasi, S., Saeidi, M., & Ezzati, P. (2018). Barriers for the referral to outpatient cardiac rehabilitation: A predictive model including actual and perceived risk factors and perceived control. Annals of Cardiac Anaesthesia, 21(3), 249-254. [CrossRef]
- Starbird, L. E., DiMaina, C., Sun, C.-A., & Han, H.-R. (2019). A Systematic Review of Interventions to Minimize Transportation Barriers Among People with Chronic Diseases. Journal of Community Health, 44(2), 400-411. [CrossRef]
- Syed, S. T., Gerber, B. S., & Sharp, L. K. (2013). Traveling towards disease: transportation barriers to health care access. Journal of Community Health, 38(5), 976-993. [CrossRef]
- Tessler, J., & Bordoni, B. (2021). Cardiac Rehabilitation. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK537196/.
- Turk-Adawi, K., Supervia, M., Lopez-Jimenez, F., Pesah, E., Ding, R., Britto, R. R., . . . Grace, S. L. (2019). Cardiac Rehabilitation Availability and Density around the Globe. EClinicalMedicine, 13, 31-45. [CrossRef]
- Turk-Adawi, K. I., Terzic, C., Bjarnason-Wehrens, B., & Grace, S. L. (2015). Cardiac rehabilitation in Canada and Arab countries: comparing availability and program characteristics. BMC Health Services Research, 15, 1-10. [CrossRef]
- World Health Organisation. (2021). Cardiovascular Diseases (CVD). Retrieved from https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds).
- Yohannes, A., Doherty, P., Bundy, C., & Yalfani, A. (2010). The long-term benefits of cardiac rehabilitation on depression, anxiety, physical activity and quality of life. Journal of Clinical Nursing, 19, 2806-2813. [CrossRef]
- Yuan, G., Shi, J., Jia, Q., Shi, S., Zhu, X., Zhou, Y., . . . Hu, Y. (2021). Cardiac Rehabilitation: A Bibliometric Review From 2001 to 2020. Frontiers in Cardiovascular Medicine, 8(469). [CrossRef]
| Study title | Author/year/ country | Design | Study subjects (n) | Barriers/Parameters |
|
Predictors of Early and Late Enrolment in Cardiac Rehabilitation, Among Those Referred, After Acute Myocardial Infarction |
(Parashar et al., 2012) USA |
Prospective cohort study | 1568 | demographic factors comorbidities Patient’s education level Cost of care |
|
Smoking and Cardiac Rehabilitation Participation: Associations with Referral, Attendance, and Adherence |
(Gaalema et al., 2015) USA |
Systematic review | 56 peer-reviewed articles | comorbidities |
|
Factors Associated with Utilization of Cardiac Rehabilitation Among Patients With Ischemic Heart Disease in the Veterans Health Administration |
(Schopfer et al., 2016) USA Qualitative study |
56 patients, providers, and CR program managers |
Lack of provider knowledge of the benefits and guidelines Inter-provider communication Cost-of care Travel/distance Lack of patient desire |
|
|
Association of Mental Health Conditions With Participation in Cardiac Rehabilitation |
(Krishnamurthi et al., 2019) USA Prospective cohort study |
86 537 patients | Comorbidities | |
|
Barriers for the Referral to Outpatient Cardiac Rehabilitation: A Predictive Model Including Actual and Perceived Risk Factors and Perceived Control |
(Soroush et al., 2018) Iran Cross-sectional study |
312 CABG patients | demographic factors employment status accessibility |
|
|
Factors associated with non-attendance at exercise-based cardiac rehabilitation Retrospective cohort study |
(Borg et al., 2019) Sweden |
31,297 | comorbidities employment status accessibility |
|
|
Association of Neighborhood Socioeconomic Context With Participation in Cardiac Rehabilitation Prospective cohort study |
(Bachmann et al., 2017) USA |
4096 | income educational status demographic factors comorbidities |
|
|
Effect of cardiac rehabilitation referral strategies on utilization rates Prospective cohort study |
( Grace et al., 2011) Canada |
1809 | Referral strategies | |
|
Cardiac Rehabilitation Availability and Density around the Globe Cross-sectional study |
(Turk-Adawi et al., 2019) Global |
98 countries | CR availability Referral strategy Mode of delivery |
|
|
Cardiac rehabilitation delivery in low/middle-income countries Cross-sectional study |
(Pesah et al., 2019) Global |
55 countries | Availability Core components of the program Cost of care |
|
|
Physician-Related Factors Affecting Cardiac Rehabilitation Referral Cross-sectional study |
(Moradi et al., 2011) Iran |
122 Cardiologists |
Physician’s knowledge about CR | |
|
Referral and participation in cardiac rehabilitation of patients following acute coronary syndrome; lessons learned Retrospective cohort study |
(Rodrigo et al., 2021) Netherland |
469 | Accessibility Comorbidities |
|
|
Predictors of Enrollment in Cardiac Rehabilitation Programs in Spain Retrospective cohort study |
( Chamosa et al., 2015) Spain |
756 | Demographic factors Comorbidities accessibility |
| Author/ Year | Themes | Results | Interpretation of significant findings |
| Healthcare system-related factors | |||
|
(Turk-Adawi et al., 2019) ( Pesah et al., 2019) |
Availability of CR programs |
CR was available in 111/203 countries. Availability by region shows significant difference (p < .001) 5753 programs globally (χ2 =37.3, p<0.001) |
CR is available in 54.7% of countries worldwide 80.7% of countries in Europe, to 17.0% in Africa Could serve 1,655,083 patients/year, despite an estimated 20,279,651 incident IHD cases globally/year CR is only available in 16.7% of LICs, 47.1% of MICs, and 86.2% in HICs There was one CR spot for every 66 IHD patients in LMICs (vs 3.4 in HICs) |
|
(Grace et al., 2011) (Turk-Adawi et al., 2019) |
Referral strategies |
(OR,3.27; CI, 1.52-7.04) (OR,3.35; CI, 1.54-7.29) (OR,8.41; CI, 3.57-19.85) (OR,1.36; CI, 1.35-1.38) |
Automatic referral strategy resulted in 70.2% referral rate and 60% of enrollment in CR Liason referral strategy resulted in 59% referral rate & 50 % enrollment Combined use of automatic & Liason strategies resulted in 85.8% referral rate & 73.5% enrollment Traditional referral strategy resulted in a 32.2% referral rate & 29% enrollment Systematic referral strategies resulted in 36% higher referral rates compared to traditional referral strategies. |
|
(Schopfer et al., 2016) (Moradi et al., 2011) |
Providers’/ physicians’ knowledge | 73% - CR providers 79.5% - cardiologists |
73% of CR providers perceived lack of knowledge regarding the benefits and guidelines causes fewer referral rates to CR 79.5% of cardiologists perceived low general knowledge about CR programs as the standard of care impact on referral to CR |
|
(Schopfer et al., 2016) |
Inter-provider communication | 18% - CR providers 17% - CR managers |
18% of CR managers and 17% of providers perceived poor communication between clinicians regarding patients' eligibility to CR resulted in fewer referrals |
| (Turk-Adawi et al., 2019) | Mode/setting of delivery | (OR = 1.05, 95%CI = 1.04–1.06) | CR programs offered individualized consultation with physicians reported high participation rates and residential programs reported higher patient compliance |
| Socioeconomic factors | |||
|
(Parashar et al., 2012) (Bachmann et al., 2017) (Soroush et al., 2018) |
Level of education |
1st month(OR, 1.38; 95% CI, 1.04–1.84) After 6 month (OR, 1.81; 95% CI, 1.42–2.30 Complete high school-(OR 1.20; 95% CI,0.92-1.58) Complete college- (OR 1.61, 95% CI, 1.06–2.44) Illiterate -7% Less than diploma-9% Academic -16% |
People who have at least high school education have 38% higher participation at 1st month and 81% after 6 months of AMI People who have completed college has 61% higher participation in CR compared to people who completed high school Higher referral rate(16%) for CR among people who complete academic education |
|
(Parashar et al., 2012) (Pesah et al., 2019) (Schopfer et al., 2016) |
Cost of care |
Uninsured(first month) (OR, 0.39; 95% CI, 0.21–0.71) After 6months insured vs uninsured p<0.001 Economic burden(first vs 6th months) (OR, 1.48; 95% CI, 0.97-2.26). Vs (OR, 0.56; 95% CI, 0.38–0.81) LMICs vs HICs Out-of-pocket(n=212, 65.0%) vs(n=184, 24.9%) 27% of participants perceived cost of care as a barrier |
Uninsured patients were 40% less likely to participate in the first month and no significance in insured vs uninsured at 6 months Patients with economic burden showed 48% of higher participation in the first month but 44% of less participation at 6 months High out-of-pocket expenditure was significantly associated with less participation and high dropout rates in LMICs compared to HICs. 27% perceived higher cost of CR program reduce participation |
|
(Soroush et al., 2018) (Borg et al., 2019) (Chamosa et al., 2015) (Bachmann et al., 2017) |
Employment status/income |
Employed 23% personal job 6.6% retired 12% unemployed 3.7% employed vs retired(OR 0.86;CI,0.80-0.93) self-employed(OR=1.56; 95% CI: 0.62-3.92) retired (OR = 1.33; 95% CI: 0.62-2.77). <$15,000 vs >$25,000 (OR 1.68, 95% CI, 1.17–2.42) |
unemployed, retired, or self-employed patients were less likely to be referred to CR than employed patients. Retired patients are 14% less likely to participate in CR Both self-employed(56%) and retired patients(33%) have higher enrollment Household income >$25,000/yr has 68% higher participation |
|
(Schopfer et al., 2016) (Soroush et al., 2018) (Rodrigo et al., 2021) (Borg et al., 2019) (Chamosa et al., 2015) (Bachmann et al., 2017) |
Accessibility to CR facilities |
68% respond to travel issues as a barrier Distance to CR e]center (p<0.042) <5km vs. > 20 km referral(OR 4.0; CI1.26–13.0) participation(OR 0.2, CI 0.07–0.79, (OR 1.75 [95% CI: 1.64–1.86] (OR = 2.87; 95% CI: 1.29-6.41) (OR 0.71, 95% CI, 0.59–0.84) |
The most perceived barrier to CR participation is long distance and transportation issues Larger distance was significantly associated with less referral Larger distance(>20km) to CR centers has 4 times higher referral rate but their participation in CR is significantly low Distance >16km increase the non-attendance by 75% Distance to CR unit >50km causes 3 folds more likely to CR non-enrollment Distance increase to CR centers from 3.8km to 25 km reduce the attendance by 29% |
| Individual characteristics | |||
|
(Parashar et al., 2012) (Chamosa et al., 2015) |
Age |
OR, 0.85 for each 10-year increment; 95% CI, 0.74–0.97 (OR = 1.05; 95% CI: 1.02-1.09). |
Older patients are 15% less likely to participate in CR Age was associated with no enrollment, with the chance of not enrolling increasing by 5% for every year of age |
|
(Parashar et al., 2012) (Borg et al., 2019) (Chamosa et al., 2015) |
Gender |
( OR, 0.61; 95% CI, 0.44, 0.86) (female vs male) OR, 0.85; 95% CI,0.80,0.90 Female vs male (20.8% vs 35.9%) Women with MI(OR, 6.35; CI, 2.53-11.81) |
Women 40% less likely to participate in CR Male were 15% less likely to participate Referral was less among women Women with MI has 35% higher non-participation |
|
(Parashar et al., 2012) (Borg et al., 2019) ( Krishnamurthi, Schopfer, Shen, & Whooley, 2019) ( Chamosa et al., 2015) (Gaalema et al., 2015) (Bachmann et al., 2017) |
Comorbidities |
hypertension (OR, 0.58; 95% CI, 0.43–0.78), PAD (OR, 0.43; 95% CI, 0.22–0.85), and previous PCI (OR, 0.55; 95% CI,0.36–0.83), Smokers (OR, 0.59; 95% CI,0.44–0.80) Diabetes (OR,1.20; 95% CI, 1.13-1.28) Hypertension (OR,0.94; 95%CI, 0.89-0.98) Smoking (OR, 1.63; 95% CI,1.54-1.74) (OR, 1.57; 95% CI, 1.43–1.74) (OR: 6.35; 95% CI: 2.53-11.81). (OR, 0.59; 95% CI, 0.44–0.80 (OR 0.65, 95% CI, 0.49–0.85,). |
Patients with a greater number of comorbidities were less likely to participate in CR non-attendance at CR was higher for individuals with a higher burden of comorbidities and for smokers Patients with both PTSD and depression had a 57% greater odds in participating in CR than those without depression or PTSD women with previous MI less likely to participate smokers were less likely to participate Smokers were 35% less likely to participate in CR programs |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





